This advertorial is sponsored by Laminate Medical.
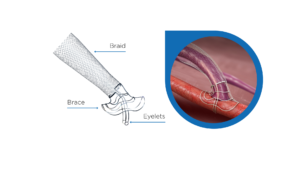
The VasQ extravascular support device (Laminate Medical) is designed to address haemodynamic and mechanical factors of arteriovenous fistula (AVF) failure, offering fewer interventions, and better long-term durability than traditional fistulas. This is according to an expanding evidence base, which now includes 18-month data from Tan Tock Seng Hospital in Singapore. Senior author Enming Yong and co-author Li Zhang speak to Vascular News about what these latest findings mean for vascular access patients.
Yong, Zhang and colleagues’ newest publication, by Lim et al, published in the Journal of Vascular Access (JVA) last year, was intended to address vascular access challenges specific to the patient population they serve. “We have a high burden of end-stage renal disease (ESRD) patients in Singapore,” Yong notes, specifying that Tan Tock Seng Hospital is a high-volume access centre. “Every surgeon does about 80–100 access surgeries a year.”
The publication’s 18-month data demonstrates that VasQ improves and sustains the life of healthy fistulas.1 In particular, the authors highlight positive outcomes regarding early physiological maturation, durable access, and primary patency, as well as a strong safety profile. The study reviewed 118 consecutive patients who had the VasQ device implanted during surgical AVF creation from October 2023 to February 2025 at two tertiary referral centres in Singapore. The majority of AVFs created with the device (57.6%) were radiocephalic (RC) fistulas, 33.9% were brachiocephalic (BC) fistulas, and 8.4% were brachiobasilic transposition (BVT) fistulas.
Outlining the results, Yong, Zhang and colleagues note in JVA that AVF physiological maturation was 64.4%, 83.1%, and 95.8% at one, three, and six months, respectively. In addition, they share that the overall balloon-assisted maturation (BAM) rate was 26.9%, down from 46%; there were four (3.9%) instances of haemodialysis access-induced distal ischaemia; and there were no device-related complications nor infections during the follow-up period.1,2
Furthermore, the authors write that primary patency was 62.5%, 49%, and 37.3% at six, 12, and 18 months, respectively, while secondary patency was 98.3%, 88.4%, and 86.2% at the same timepoints. “Comparatively,” they note, “previous retrospective series in our centre demonstrated a primary failure rate of 25% with RC AVFs and primary patency rates of 33% and secondary patency rates of 72% at 12 months without the use of [the] VasQ device.”
“The VasQ device demonstrated safety and efficacy with improved AVF maturation in a realworld Asian population, across all AVF types (RC, BC, and BVT),” the authors conclude, adding that the rate of primary failure was low while the BAM rate improved compared to the team’s historical data. As a result, the authors “recommend [the] VasQ device as standard of care in patients undergoing AVF creation”. Yong is set to present these data at the 2026 Charing Cross (CX) Symposium (21–23 April, London, UK).

In conversation with Vascular News, Yong and Zhang delve into the rationale behind the study, highlighting the team’s aim of replicating existing results from the USA and Europe in an Asian population.
Literature highlights on the VasQ so far include the US pivotal trial, results of which were shared in 2023 in the Journal of Vascular Surgery (JVS).3 In this paper, Ellen Dillavou (Triangle Vascular Associates, Durham, USA) and colleagues conclude that VasQ “shows great promise in expeditiously and efficiently enhancing AVF functional success.” More recently, in JVA, Robert Shahverdyan (Vascular Institute, Hamburg, Germany) and colleagues reported positive fiveyear results from their European single-centre experience.4 “There are many papers from around the world, single-centre and multicentre services, all showing a positive benefit, and we wanted to show in our own study population whether [VasQ] was also applicable,” says Yong. “I think we’re reasonably convinced that [the device] works in an Asian context, despite smaller blood vessels, different demographics.”
Specifically, in discussion of the latest findings, Yong comments on his reduced BAM and fistuloplasty rates. He also highlights the added benefits seen when the anastomosis is supported. “When the patients do get stenosis,” he says, “it’s not so severe and is isolated to the anastomotic area”. Zhang points out another key benefit she has anecdotally observed, which is that the device can be “useful in patients with very deep anatomy”.
Yong also remarks that the advantages of VasQ can be seen both intra- and postoperatively. Immediately following a procedure, from his observations, he believes that VasQ’s support helps prevent haematoma and early failure. In addition, Yong states that the VasQ makes the longer-term postoperative course “a lot more predictable in terms of what the surgeon can expect”, highlighting fewer instances of severe stenosis that require intervention.
Yong and Zhang share that they have incorporated VasQ into their practice as standard of care in the last two years. “In our centre, we have already had quite a lot of experience and so we embrace this new technology,” says Yong. Zhang is in agreement, noting that “so far, we have not observed any adverse events”.
Yong does highlight a small learning curve with VasQ. However, he shares, “the on-site support from both our local distributor and also by Laminate has been quite fantastic”. Yong also mentions his visit to Shahverdyan’s centre in Hamburg for additional training. Overall, Yong relays that the Singapore team has “found [VasQ] to be very effective clinically”.
In terms of what further evidence is needed, Yong highlights the importance of collecting outcomes regarding the cost-effectiveness of VasQ. Indeed, this is forthcoming, with a quality improvement report that includes a cost-effectiveness analysis—incorporating data from both the USA and Europe—in the works.
Zhang adds that there may be some benefit of the VasQ in preventing a brachial artery-based fistula from developing steal syndrome, while noting that more data are needed to validate this observation.
On this point, Yong relays the team’s hope to eventually look into outcomes for brachial artery-based fistulas besides the steal syndrome rate. “I personally believe that having the VasQ there may also limit the severity of cephalic arch stenosis,” he remarks, referencing the impact of VasQ on flow rate and haemodynamic profile.
For now, Yong, Zhang and colleagues’ latest study adds to a growing body of evidence on the clinical impact of the VasQ across the globe. “There are so many positive studies about [the VasQ],” Yong concludes, “so I encourage anyone, if you think that it may be useful to your practice, to try it.”
References
- Lim X, Zhang L, Pan Y, et al. J Vasc Access 2025 Oct; Online ahead of print.
- Yong E. Asian Society for Vascular Surgery annual congress 2024.
- Dillavou E et al. J Vasc Surg 2023; 78(5):1302-12.
- Shahverdyan R et al. J Vasc Surg 2025 Jul;82(1):229-39. Epub 2025 Jun 4.
Prior to use, please reference the Instructions for Use for more information on indications, contraindications, warnings, precautions and adverse events available at https://laminatemedical.com/eIFU