The results of AVeNEW, the first level one clinical study dedicated solely to the use of a covered stent designed to treat stenosis in the arteriovenous (AV) fistula access circuit, show that the Covera vascular covered stent (Bard) demonstrates “significantly better” target lesion primary patency compared to percutaneous transluminal angioplasty (PTA) at six months, with the difference sustained in the 12-month data, and better access circuit patency was maintained at 12 months.
Lead investigator Bart Dolmatch, (The Palo Alto Medical Foundation, Mountain View, USA) recently presented this “first look” at the 12-month results of the AVeNEW study at the annual meeting of the Cardiovascular and Interventional Radiological Society of Europe (CIRSE 2019; 7–11 September, Barcelona, Spain).
Dolmatch and colleagues describe AVeNEW as a prospective, international, multicentre randomised controlled clinical trial, designed to assess the Covera vascular covered stent compared to angioplasty for the treatment of stenotic lesions in the venous outflow of upper extremity AV access circuits in patients dialysing with an autogenous fistula.
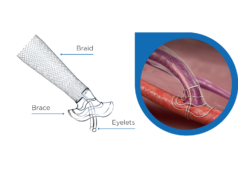
The Covera stent, which received US Food and Drug Administration (FDA) approval in July 2018, is described on the FDA website as “an expandable, flexible, metal [nitinol] tube covered with a material called expanded polytetrafluoroethylene [ePTFE].”
Dolmatch and colleagues comment that AVeNEW is “the first level-one clinical trial dedicated solely to the use of a covered stent graft designed to treat stenosis in the AV fistula access circuit,” and they conclude that the covered stent group demonstrated “significantly better” target lesion primary patency compared to the PTA group at six months, with the difference sustained at the 12-month data. Access circuit primary patency was numerically different at six months, and “statistically better” for the stent graft group at 12 months.
The investigators enrolled 280 patients with stenosis ≥50 per cent in the venous outflow of the AV access circuit, and with clinical or haemodynamic evidence of fistula dysfunction, at 20 centres across the USA, Europe, Australia, and New Zealand.
They detail that patients received either PTA alone or PTA followed by covered stent placement. The primary endpoints were six-month target lesion primary patency and 30-day safety. Secondary outcomes included target lesion primary patency at 12 months, and access circuit primary patency at six and 12 months.
The majority of patients included in the study were Caucasian (68.6%) with a mean age of 63±12.4 years, and most patients were male (61.8%). Patients included in the study had multiple risk factors for renal dysfunction, including diabetes mellitus (69.6%) and hypertension (97.1%). Lesions were restenotic in 73.2% of cases, were on average 29.3±17.2mm long (diameter stenosis: 72.5±12.5%), and 53% were in the cephalic vein arch.
The proportion of patients free from a primary safety event with the covered stent (95%) was non-inferior to PTA (96.4%) at 30 days (p=0.002, significant for non-inferiority). Target lesion primary patency was significantly better for the covered stent group (78.7%) versus the PTA group (47.9%) at six months (Kaplan-Meier analysis) and remained statistically significant at 12 months (57.5% vs. 21.2%, respectively; p<0.001). Access circuit primary patency at six months numerically favoured the covered stent (50.7%) group compared to the PTA group (43.8%) while at 12 months the difference was statistically significant (28.9% vs. 17.7%, respectively; p=0.016).
The investigators summarise that the results of the AVeNEW study have shown that the covered stent conferred more than a 30% improvement in patency at the target lesion compared to PTA at both six and 12 months. Furthermore, the covered stent group had statistically superior access circuit patency at 12 months. “Clinical follow-up is ongoing,” they comment, “and will continue out to three years”.