The first patients have been enrolled in the US FDA pivotal study of VasQ (Laminate Medical Technologies), an implanted blood vessel external support device for patients requiring arteriovenous fistula as vascular access for haemodialysis.
The first surgeries were performed by Jason Burgess and Paul Orland at the Carolinas Medical Center-Mercy, Charlotte, USA.
“We are excited to be the first site that enrolled patients in the USA. The device was easy to implant and I am happy with the surgical results. We are looking forward to evaluating the device’s long-term effect,” says Burgess.
“The device was easy to handle and I was very happy with the postoperative results. This new technology is targeting the major problems of AVFs: maturation and long-term longevity of the fistula,” says Orland.
The prospective, multicentre, single-arm, open-label, 13-site study will enrol 129 male and female patients, 18 to 80 years old, who require creation of new brachiocephalic fistula. During screening, surgeons will assess additional eligibility criteria such as adequate blood vessel anatomy and absence of potentially precluding past and current medical conditions and comorbidities. The primary effectiveness endpoint for this trial will be the primary patency rate six months after creation of the arteriovenous fistula. Patients will be followed for a total of two years.
“The launch of this pivotal study marks an important step forward for VasQ in the US market and a promising milestone for patients with kidney failure. We were excited to see the high level of interest and support from our partner sites, when we offered them to participate in the study,” says Laminate CEO Tammy Gilon.
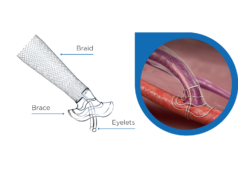
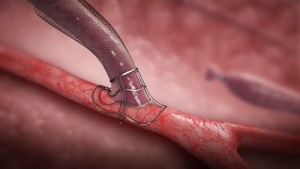
Developed by Laminate, VasQ is intended for patients suffering from kidney failure and in need of dialysis, which requires vascular access. The most common and preferred method of vascular access is an arteriovenous fistula, created by surgically suturing a blood vessel connection between an artery and a vein, usually in the region of the wrist or the elbow. Two intravenous needles are inserted through the vein to remove the patient’s blood for filtration in the dialysis machine, and then return it. This connection ensures a sufficiently high transfer of blood volume (veins do not transfer sufficient volume, while arteries are too deep for repeated insertion of a needle).
Unfortunately, a venous blockage forms in more than half of these cases. In response to increased pressure, the vein wall thickens, which in turn affects the blood flow during dialysis. As a result, the patient must have repeat interventions to save the fistula or, in cases where the fistula cannot be used, use other vascular access alternatives affecting the ability to receive dialysis and creating a burden on the hospital’s resources.
VasQ is an external scaffold placed over the fistula, creating an optimal geometric configuration with the artery and reducing the tension in the vein. This allows proper blood flow during dialysis while reducing vein blockage created by thickening of the vein wall. Studies show VasQ has significant success. VasQ is a CE marked device already in use in hospitals in Europe and in Israel.