In a Gore-sponsored Satellite Symposium at the Charing Cross Symposium (CX; 19–22 April, online), Michele Piazza (Padua, Italy) moderated a discussion on occlusive Iliac artery pathology, covering guidelines, treatment algorithms, and current knowledge gaps.
Manuel Alonso Perez (Oviedo, Spain) first delivered a presentation entitled “Treatment approach for iliac occlusive disease: What is the best option? Experience and data”. “As everybody knows, open surgery is still the gold standard for treatment of extensive aortoiliac occlusive disease,” he said. “However, nowadays, more and more type C and D lesions are treated with covered stents, mainly self-expanding covered stents.”
He told the CX audience that while bare stents are associated with a lower patency rate for complex occlusive lesions, there is no evidence on the role of the different types of covered stents (balloon-expandable covered stents vs. self-expanding covered stents) due to a lack of comparative data.
“[The] self-expanding Viabahn stent [Gore] may be the best option for external iliac artery and long iliac occlusions if there is no severe calcification,” Perez concluded. “The Viabahn balloon-expandable stent associated with the self-expanding Viabahn stent can allow for treatment of complete iliac occlusions or kissing stent technique.”
He finished by saying that new studies are needed to determine comparative and long-term results.
Case presentations
Lukasz Dzieciuchowicz (Poznan, Poland) next took to the virtual podium to present his experience in treating occlusive iliac artery pathology. He talked through the case of a 57-year-old man who presented with Rutherford III intermittent claudication. Pre-procedural angiography revealed the patient had stenosis of the terminal part of the abdominal aorta, critical stenosis of both common iliac arteries and the external iliac artery, as well as occlusion of the proximal part of both internal iliac arteries and a wide and patent inferior mesenteric artery.
“The plan was to perform a percutaneous endovascular reconstruction of the aortic bifurcation and the common iliac arteries with balloon-expandable covered stents, preserving the inferior mesenteric artery, because we believed this vessel was very important for the blood supply to the pelvis,” Dzieciuchowicz said.
The procedure was performed under general anaesthesia in a hybrid operating room. Vascular access was obtained by percutaneous puncture of both common femoral arteries and the introduction of an 8Fr introducer sheath. The patient was heparinised and posterior-anterior arteriography confirmed the presence of stenosis of the distal part of the abdominal aorta, and critical stenosis of both common iliac arteries, as well as occlusion of proximal parts of the internal iliac arteries. Arteriography in lateral projection confirmed the presence of a wide and patent inferior mesenteric artery, and stenosis of the terminal part of the abdominal aorta.
An aortic covered stent was introduced through the right common femoral artery and deployed in the aorta just below the take-off inferior mesenteric artery. Next, two Viabahn balloon-expanding stents (8x79mm) were introduced and deployed in the aortic bifurcation and common iliac arteries in a “kissing stent” configuration.
A control retrograde arteriography of the right iliac axis showed a “satisfactory” angiographic result, Dzieciuchowicz relayed. Using the same imaging modality for the left iliac axis, the proceduralists saw significant stenosis of the left external iliac artery. “This was successfully treated by the implantation of a self-expanding bare metal stents in the left external iliac artery,” the CX audience heard.
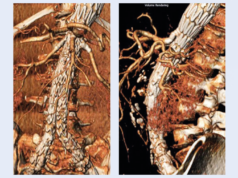
The postoperative course was uneventful, and the patient was discharged home the next day. One month after the procedure, the patient was asymptomatic. A control angiography CT showed patency of the Viabahn balloon-expandable stents without compression, as well as patency of the inferior mesenteric artery and external iliac artery stent.
“In conclusion, we may say that Viabahn balloon-expandable stents allow us to safely and effectively treat a complex aorto-iliac occlusive pathology through a standard percutaneous approach.”
Alexander Oberhuber (Dusseldorf, Germany) reached a similar conclusion following his presentation of a case of Viabahn balloon-expandable stent implantation in aortoiliac occlusive disease. In this example, a 62-year-old man with Rutherford category IV intermittent claudication, who was only able to walk a few metres before his intervention, treatment with the Viabahn balloon-expandable stent led to “a really good result”, with no residual stenosis and “very good flow” to both external iliac arteries and to both legs.
“There is no kink or compression of the Viabahn balloon-expandable stent on both sides,” Oberhuber noted, showing post-procedural angiography images.