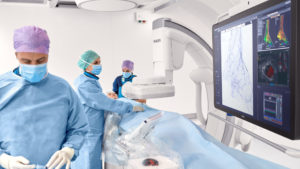
Royal Philips today announced the results of a new large-scale, real-world analysis of Centers for Medicare & Medicaid Services (CMS) data on the health outcomes of peripheral vascular interventions guided by intravascular ultrasound (IVUS).
The study was conducted independently by the Smith Center for Outcomes Research at Beth Israel Deaconess Medical Center (Boston, USA), with the results presented at Transcatheter Cardiovascular Therapeutics (TCT) 2021 (4–6 November, Orlando, USA) by Eric A Secemsky, director of vascular intervention and interventional cardiologist at Beth Israel Deaconess Medical Center and assistant professor of medicine at Harvard Medical School in Boston, USA. The study was supported by Philips.
A press release details that numerous prospective studies have already shown the benefit of IVUS guidance in peripheral vascular interventions, making it a gold-standard imaging modality for this application. The new study results now show that the outcome observations from these prior studies apply directly to a broader patient population and across vascular beds, demonstrating strong support for the use of IVUS during peripheral interventions, the release continues.
“The results of this large-scale study demonstrate favourable long-term outcomes in peripheral vascular interventions when IVUS is used,” said Secemsky. “This analysis, combined with the recent appropriate use consensus on IVUS that was presented at VIVA [Vascular Interventional Advances; 5–7 October, Las Vegas, USA], highlights a clear opportunity to improve health outcomes for millions of patients by broader and more routine implementation of the technology in clinical practice. This is a moment for us to further our efforts in saving lives and saving limbs.”
Peripheral arterial disease (PAD): A 32% reduction in major adverse limb events, including amputations, during lower extremity arterial interventions
The study looked at Medicare beneficiaries aged 65 years or older who underwent lower extremity arterial interventions between 1 January 2016 and 31 December 2019. Among 697,794 interventions, the investigators found a 32% reduction in major adverse limb events, such as amputations, over a median 425 days of follow-up. These findings were consistent across disease states, including chronic limb-threatening ischaemia (CLTI) and non-CLTI, as well as arterial segments such as iliac, femoropopliteal and tibial.
Chronic venous disease (CVD): A 31% reduction in repeat intervention, hospitalisation or death during iliofemoral venous stenting
Separately, the investigators examined Medicare beneficiary data for patients treated between 1 January 2017 and 31 December 2019 in multiple clinical settings, including hospital in-patient settings, hospital outpatient centres and private office-based clinics, involving 20,984 individual patients. Of these, 72% underwent stenting guided by IVUS. When IVUS was used, there was a 31% reduction in the composite outcome of repeat intervention, hospitalisation or death. In addition, IVUS use reduced the risk of stent thrombosis, embolisation and stenosis.
“We commend Dr Secemsky and the Smith Center for Outcomes Research for this ongoing study to simplify clinical procedures and improve clinical, economic and patient outcomes,” said Chris Landon, senior vice president and general manager Image Guided Therapy Devices at Philips. “We are committed to supporting evidence-based medical guidelines in pursuit of better patient outcomes. We believe that the ability of IVUS to deliver procedure optimisation and confidence enhances patient and staff experiences and lowers cost of care.”
First-ever global consensus for the appropriate use of IVUS in peripheral vascular disease interventions
In October 2021, a team of clinical experts led by Secemsky established the first-ever global, cross-specialty expert consensus for the appropriate use of IVUS in peripheral vascular disease interventions. This initiative was jointly supported by Philips and Boston Scientific. Today, healthcare providers’ use of IVUS in peripheral vascular disease interventions is not standardised and is therefore inconsistent. The new appropriate use expert consensus may help establish global standards of care to adopt into guidelines and improve quality of care in peripheral vascular disease, a Philips press release states.













Nice article.tha