Against the backdrop of increasing end-stage renal disease (ESRD) prevalence in the USA, Bart Dolmatch (Portola Valley, USA) presented the 24-month results of the prospective, randomised controlled AVeNEW study at the Cardiovascular and Interventional Radiological Society of Europe (CIRSE) 2020 Symposium (12–15 September, virtual).
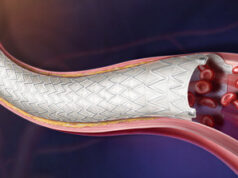
This is the first level one trial dedicated solely to assess the safety and efficacy of the Covera (BD) covered stent designed to treat stenosis in the arteriovenous fistula (AVF) access circuit. The two-year results showed statistically superior target lesion primary patency and AVF circuit primary patency with the use of the covered stent compared with angioplasty alone.
Renal replacement is expensive, online attendees of the FIRST@CIRSE session heard, and largely achieved with haemodialysis using an arteriovenous AVF. However, Dolmatch explained how AVF stenosis interferes with efficient haemodialysis, leading physicians to try and find a treatment modality that reduces its occurrence.
“Angioplasty has been our go to for many years,” he said, “but we know that the durability after angioplasty is OK, but the question is, can we improve upon angioplasty durability when treating fistula stenosis?”
Enter the AVeNEW study, a prospective, multicentre, multinational clinical trial of 280 patients with stenotic AVFs and clinical AVF dysfunction. Patients were randomised 1:1 to either the percutaneous transluminal angioplasty (PTA) group, or the angioplasty with Covera covered stent group.
The study met both its primary safety and efficacy endpoints: freedom from a primary safety event out to 30 days, and target lesion primary patency at six months, respectively. There was no significant difference in freedom from a primary safety event out to 30 days between the covered stent cohort and the angioplasty alone cohort (95% and 96.4%, respectively; p=0.002). Target lesion primary patency at six months was “superb” and “statistically superior” in the covered stent group compared to angioplasty (78.7% and 47.9%, respectively; p<0.001).
A 12-month exploratory subgroup analysis of target lesion primary patency revealed that, regardless of certain lesion characteristics, “a preferential, better outcome using the covered stent compared to angioplasty alone. A Kaplan-Meier plot showed that the freedom from loss of target lesion primary patency was superior shortly after implantation of the covered stent compared to angioplasty, and remained statistically better at all time points, with more than a 30% better patency at 24 months.
Secondary outcomes were also better for the covered stent cohort, Dolmatch related. The index of patency function and mean access circuit reinterventions were both superior in the covered stent group, while secondary patency was the same in both groups (91.4%). “Interestingly, all-cause death was lower in the covered stent group than the angioplasty group,” Dolmatch continued. “I am not sure if this is statistically significant, we have not done that analysis yet, but it is a curious finding.”
Looking specifically at freedom from loss of access circuit primary patency, he commented: “Access circuit patency for an AVF drops off regardless of which group you are in, and yet, at 24 months, there is a statistically superior outcome of circuit patency for the covered stent group compared to the angioplasty group [p=0.02].”
The AVeNEW trial is still ongoing, with one more year of data collection and analysis ahead, to bring its total duration to three years.