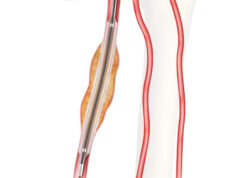
Bard’s Lutonix 035 drug-coated balloon PTA catheter (DCB) has been granted premarket approval (PMA) by the US Food and Drug Administration (FDA) for a new indication and is now available for sale in the USA.
With this approval, the Lutonix 035 DCB catheter becomes the first and only drug coated balloon that is FDA approved as safe and effective in end-stage renal disease (ESRD) patients with stenotic lesions in dialysis arteriovenous (AV) fistulae, a Bard press release says. This latest approval adds to the prior FDA indication of the DCB for the treatment of superficial femoral artery and popliteal artery disease.
The FDA approval was based on the results of the LUTONIX AV clinical trial, the first investigational device exemption trial using DCBs in patients with stenotic lesions in AV fistulae. The follow-up results from randomised patients who were treated with the Lutonix DCB catheter demonstrated safety comparable to uncoated balloons.
The Lutonix 035 DCB also demonstrated a sustained clinical benefit compared to conventional angioplasty through 12 months:
- 71.4% target lesion primary patency (TLPP) at 180 days with superior results at 210 days (DCB 64.1% vs. PTA 52.5%);
- 31.3% fewer reinterventions compared to PTA at six months;
- Nearly two months more reintervention-free days (217 days vs. 163 days) compared to PTA;
- 31.2% improvement in TLPP through 12 months;
- 95% freedom from primary safety event, indicating a consistent safety profile to PTA.
“For patients undergoing haemodialysis for kidney failure—who already spend a significant portion of their time undergoing dialysis and other treatments—repeated reinterventions to maintain AV access can be an added burden, with many patients returning as frequently as every other month,” said Scott O Trerotola (Perelman School of Medicine, University of Pennsylvania), principal investigator of the LUTONIX AV clinical trial. “The Lutonix 035 DCB provides another option for physicians. It is intended to offer patients with end-stage renal disease fewer interruptions in treatment and less time undergoing access maintenance, potentially leading to improved patient satisfaction and quality of life.”