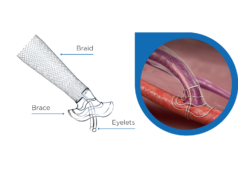
VasQ, a high haemocompatibility biosynthetic vascular device from Laminate Medical Technologies, could be protective against the haemodynamic modifications that occur during arteriovenous fistulae (AVF) creation, a recent article in The Journal of Vascular Access reports. Roberto Palumbo (Saint Eugenio Hospital, Rome, Italy) and co-authors caution that their results, which derive from their clinical experience and are thus representative of a “real-life setting”, should be considered preliminary. They call for further research of the VasQ device in AVF creation, and say that “further effective treatments are needed to prevent or treat AVF failure”.
According to Palumbo et al, the VasQ device was designed “to improve the outcome of AVF [creation] by optimising the haemodynamics of the flow in the juxta-anastomotic region of the AVFs through tailored external support”. They continue: “The rationale for supporting the implantation of [the] VasQ device is based on the reduction of the turbulent blood flow through the anastomotic site and of the radial stretching of their venous wall, allowing a potential attenuation of hyperplasia and stenosis consequences and, finally, improving AVF-outcomes in haemodialysis patients.”
AVFs are the current gold standard for vascular access during the treatment of optimal chronic haemodialysis patients, due to their prolonged patency and durability, and thanks to their low complication profile. However, there is a high non-maturation rate of native fistulas. The study authors note that a prolonged maturation time, neointimal hyperplasia at the anastomotic site, and a high rate of abandonment are disadvantages associated with AVFs, and state that AVF creation “may cause significant haemodynamic modification in cardiovascular parameters”, potentially leading to adverse cardiac outcomes, such as progressive heart failure.
To establish if the use of the VasQ device would help reduce these haemodynamic modifications, the investigators compared patients who underwent native radio-cephalic AVF creation with and without implantation of the device at their institution between May and September 2019 (15 individuals in each group). Haemodynamic parameters were evaluated pre-operatively, and at one, three, and six months follow-up. The patency and complication rate were also evaluated.
At baseline, there was no significant difference between the treatment group and the control group in terms of mean preoperative arterial flow, vein diameter, preoperative ejection fraction, and cardiac output. Arterial diameter was greater in the treatment group (those where the VasQ device was deployed) at baseline (3.4±0.8mm vs. 2.8±0.5mm), but Palumbo and colleagues dismiss this, writing: “Although the vessel radius is considered a major determinant of the vessel flow, this finding may have reflected only marginally in the clinical results achieved in the VASQ device implanted [in] patients”.
While at one-month follow-up, there was no difference in mean arterial flow between the two cohorts, a significant difference was observed at three months (645±143mL/min in the VasQ group vs. 824±211mL/min in the control group; p=0.02) and six months (714±146mL/min vs. 810±194mL/min; p=0.05).
At six months follow-up, the cardiac output flow was lower in the cohort of patients implanted with the VasQ device: 4,458±928ml/min versus 5,599±1,355mL/min (p=0.05). Palumbo et al suggest that this could mean that the VasQ device “may provide a potential benefit in preventing haemodynamic modifications of the cardiovascular system and preventing the overload of the left ventricle by reducing the altered high cardiac output of haemodialysis patients associated with AVF creation”.
“Of note, no VasQ device complications were recorded,” the authors write. “The VasQ has been well tolerated by the patients, and no patient had poor subcutaneous tissues at the anastomotic site. During surgery, no technical complication occurred.”
At six months, primary patency was 73% in the treatment group and 80% in the control group, respectively. Cumulative patency was 80% and 86%, respectively, in implanted VasQ device patients compared to those in the control group.
“Although our experience is limited to a small group of patients with a relatively short follow-up”, Palumbo and colleagues write, “we confirmed the substantial safety and utility of [the] VasQ device in AVF creation. […] Our experience outlined that the implantation of [the] VasQ device during AVF creation compared to those [who underwent the] standard technique may allow a stabilisation of the high cardiac output of haemodialysis patients.”