Twelve-month data prove that intravascular lithotripsy; a novel approach using pulsatile sonic pressure waves to modify intimal and medium calcium in stenotic peripheral arteries, is a safe and effective treatment option. This is the result of the Disrupt PAD II trial, presented by Andrew Holden, Auckland Hospital, Auckland, New Zealand, for the first time at the Cardiovascular and Interventional Radiological Society of Europe annual meeting (CIRSE; 22–25 September 2018, Lisbon, Portugal).
Twelve-month data prove that intravascular lithotripsy; a novel approach using pulsatile sonic pressure waves to modify intimal and medium calcium in stenotic peripheral arteries, is a safe and effective treatment option. This is the result of the Disrupt PAD II trial, presented by Andrew Holden, Auckland Hospital, Auckland, New Zealand, for the first time at the Cardiovascular and Interventional Radiological Society of Europe annual meeting (CIRSE; 22–25 September 2018, Lisbon, Portugal).
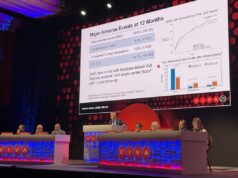
Speaking to the CIRSE audience, Holden explained that acute results were strong, with compelling safety data showing a final residual stenosis of 24.2%, with a high acute gain of 3mm and minimal vascular complications. In addition, Holden implied that the primary safety profile was “very good”, given that the only major adverse event though to 12 months was a dissection that occurred at the time of procedure.
DISRUPT PAD II was a non-randomised, multicentre study that enrolled 60 patients with complex, calcified peripheral arterial stenosis at eight sites. Patients were treated with the peripheral intravascular lithotripsy system (Shockwave Medical), and followed out to 12 months.
Calcium burden was significant, with 85% of the patient cohort exhibiting severe calcification involving both sides of the arterial wall (using the PARC definition; 50% of patients had severe calcification using the pre-defined Core Lab definition) and an average length of calcium of 98.1%.
The study investigators report high acute gain (following low pressure) in terms of the reduction of pre-procedural severity of stenosis, as well as cross-sectional area gain. This resulted in low dissections and minimal use of stents in this calcified population.
Additionally, 12-month primary patency was 54.5%, with a freedom from target lesion revascularisation rate of 79.3% in a stand-alone therapy. Primary patency outcomes were shown to improve by optimising the procedural technique: appropriate balloon sizing and intravascular lithotripsy therapeutic coverage resulted in the increased primary patency of 62.9% at 12-months follow up, with freedom from target lesion revascularisation being 91.4%.
Target lesion patency; the primary effectiveness endpoint of the study, defined as freedom from ≥50% restenosis, was found to be 69.8% (30/43 patients), as measured by duplex ultrasound. Clinically, improvements in functional outcomes were sustained through to 12-months, in terms of both the ankle-brachial index and the Rutherford score.
In conclusion, the Disrupt PAD II trial remains the first and only core lab adjudicated study to exclusively enrol and follow out to 12-months, heavily calcified lesions. Furthermore, Holden maintained that when intravascular lithotripsy is utilised as a stand-alone therapy in this complex patient population, primary patency outcomes improve.
Regarding the next steps in clinical development, Holden stated: “Importantly, the Disrupt PAD III trial is recruiting… a much larger, 400 patient trial looking to evaluate the role of intravascular lithotripsy in the setting of drug coated therapy.” Specifically, patients have been randomised to intravascular lithotripsy in combination with the IN.PACT drug coated balloon (DCB; the treatment arm) or plane balloon angioplasty and DCB (the control arm), in order to address plaque modification in heavily calcified arteries. “This will be a very important trial to establish the benefit of intravascular lithotripsy in the DCB era,” Holden concluded.