New findings from the C-GUARDIANS II study indicate that the CGuard Prime carotid stent system (InspireMD) achieves high procedural success, durable early luminal restoration, and “excellent” periprocedural safety outcomes, in patients undergoing transcarotid artery revascularisation (TCAR). This is according to data from the first 36 patients enrolled in the study, which were presented for the first time during yesterday morning’s carotid and acute stroke session at the 2026 Charing Cross (CX) Symposium (21–23 April, London, UK).
Presenter Patrick Muck (Good Samaritan Hospital, Cincinnati, USA) explained that C-GUARDIANS II is a multicentre, single-arm pivotal study designed to evaluate the safety and efficacy of the CGuard Prime (80cm) used in conjunction with the US Food and Drug Administration (FDA)-cleared Enroute transcarotid neuroprotection system (NPS; Silk Road Medical/Boston Scientific) in patients undergoing carotid artery stenting (CAS) via the TCAR approach.
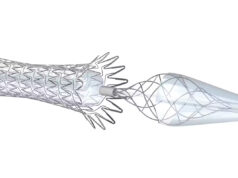
Before delving into the study details, Muck remarked on the design of the CGuard stent. “As a programme director, for years you talk to your trainees about open- and closed-cell stents. Well, this stent is actually both. It’s both wrapped into one,” he informed the CX audience.
Muck also put the C-GUARDIANS II trial in the context of other carotid trials from InspireMD. “[Christopher] Metzger already has led the C-GUARDIANS I trial, which led to the FDA approval of the 135cm CGuard Prime stent, and [Patrick] Geraghty and myself are honoured to be able to lead the C-GUARDIANS II trial. A little bit later—probably Q2, perhaps Q3—we’re going to start C-GUARDIANS III, which will include InspireMD’s proprietary SwitchGuard NPS system for TCAR,” he shared.
Muck noted that the C-GUARDIANS II study is being conducted across 11 investigational sites in the USA, with target enrolment of 50 patients now complete. He commented that the patients enrolled in the study represent a high-surgical-risk group, with ≥25% symptomatic.
In terms of patient demographics, Muck detailed that these were “pretty typical” of the population in question, homing in on the fact that 30% had prior history of stroke and 11% had prior transient ischaemic attack (TIA).
Sharing podium-first results, Muck reported a 100% acute device success rate and 97.2% technical success rate in the first 36 patients included in the study. He explained that one patient did not meet the criteria for technical success.
Moving on to secondary clinical endpoints, Muck reported no death, stroke or myocardial infarction within 30 days of procedure, as well as no stent thrombosis or device-related serious adverse events (SAEs).
In his concluding statements, Muck remarked on the “incredible results” he has seen so far, summarising that primary and secondary procedural endpoints were met, and reiterating the 100% acute device and procedural success as well as >97% technical and treatment success.
The presenter added that all 30-day clinical safety endpoints were fully achieved, with no deaths, strokes, myocardial infarctions, stent thromboses, or SAEs.
In addition, Muck noted that duplex ultrasound confirmed 100% stent patency at 30 days, with no evidence of restenosis or thrombosis, and that the device performed reliably across diverse anatomical and lesion characteristics with significant baseline stenosis.