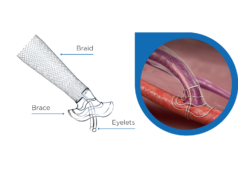
Humacyte today announced that five-year data from a phase 2 clinical trial of patients receiving the investigational Human Acellular Vessel (HAV) for arteriovenous (AV) access in haemodialysis have been published in the European Journal of Vascular and Endovascular Surgery companion journal EJVES Vascular Forum. The manuscript, entitled, “Five-year outcome in patients with end-stage renal disease who received the bioengineered human acellular vessel for dialysis access,” reports the durable long-term use and ongoing clinical function of the HAV in patients with end-stage renal disease who are undergoing haemodialysis.
In the Phase 2 long-term follow-up data, the HAV was observed to provide routine and functional haemodialysis access for patients with end-stage renal disease who require dialysis three times a week. At month 60, patency allowing for reliable dialysis access cannulation was estimated at 58.2% of evaluable patients (i.e. those who completed the original 24-month study with patent HAVs and consented to participate in the long-term follow-up; 95% confidence interval [CI], 39.2–73.1%), after censoring for deaths and withdrawals. While there was no comparator in this phase 2 trial, historical reports of arteriovenous fistula (AVF) indicate an approximately 30% functional patency of evaluable patients at five years. In addition, no infections of the HAV were reported during the five-year follow-up period, with the HAV being well tolerated and non-immunogenic.
“Patients with end-stage renal disease require chronic vascular access for haemodialysis, and those who are not candidates for fistulas must rely on synthetic arteriovenous grafts, which have a higher rate of complications including an increased risk of infection,” said Tomasz Jakimowicz (Medical University of Warsaw, Warsaw, Poland), principal investigator of the trial. “I am encouraged by the results from this trial because in addition to retaining structural integrity needed for haemodialysis, the HAV was observed to have a low risk of infection with long-term use. These results indicate the potential of the HAV as a promising option for vascular access in haemodialysis.”
“We are pleased to share these promising data, representing the longest-term follow-up of any trial of implanted bioengineered human vascular tissue and 133 cumulative patient years of HAV exposure, with our scientific peers,” said Laura Niklason, chief executive officer of Humacyte. “The data reinforce our earlier observations regarding the safety, durability and potential to become living tissue of Humacyte’s investigational engineered off-the-shelf replacement vessels. We look forward to our continued late-stage evaluation of the HAV in AV access, vascular trauma repair and peripheral arterial disease, while advancing our earlier stage work in complex tissue constructs and organ systems.”
As a follow-up to the phase 2 trial described in the publication, Humacyte is currently conducting a phase 3 trial in up to 240 dialysis patients. The Phase 3 trial is a prospective, multicentre, open-label, randomised, two-arm comparative trial designed to assess the usability of the HAV for dialysis at six and 12 months as a comparison to autogenous fistulas. As of 31 December 2021, 207 patients had been enrolled in the phase 3 trial.
Humacyte advises that the HAV is an investigational product candidate and is not currently approved for sale by the US Food and Drug Administration (FDA) or any international regulatory authority.