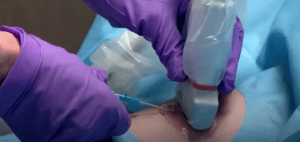
A new survey among vascular access (VA) and emergency department (ED) clinicians has revealed significant levels of variation in ultrasound-guided peripheral IV (UGPIV) practices and supply use across hospitals and alternate care settings. Published in the September issue of the Journal of the Association for Vascular Access, the findings carry critical implications for patient safety.
A total of 1,475 VA and ED practitioners responded to the survey, which was designed to gain better insight into clinicians’ current practices regarding UGPIV insertion. The survey also identified inconsistencies in supply use across hospital departments. The survey was conducted by Nancy Moureau (Griffith University, Brisbane, Australia) an internationally recognised expert and consultant in vascular access and CEO of PICC Excellence.
“Identifying gaps and variations in clinical practice forms the basis of quality initiatives intended to improve patient safety. This survey revealed clinically meaningful differences in all variables for UGPIV procedures and supplies,” said Moureau. “Aseptic technique is essential for minimising contamination, but its effectiveness is diminished if it is not done in a consistent manner. Often inconsistencies in supply usage point to variation in policy application and the potential for substandard practices. The survey results suggest a need for clinical education on the application of UGPIV guidelines, and for greater scrutiny over supplies and techniques in order to promote standardisation.”
The lack of consistency revealed by the survey is apparent in respondents’ varied use of transducer protection and gel. To minimise contamination during UGPIV insertions, current guidelines—such as those from the American College of Emergency Physicians and the American Institute of Ultrasound in Medicine—recommend use of a transducer cover and single-use gel packets (sterile or non-sterile). According to the survey, however, just 59% of VA clinicians and 11% of ED clinicians always use a sterile probe cover during UGPIV procedures, and only 64% of VA personnel and 13% of ED personnel use sterile gel. In addition, more than 22% of respondents stated that they vary between multi-use gel bottles and single-use gel packets, both sterile and non-sterile.
The survey results also highlight issues resulting from the presence of gel in the area of the sterile insertion site. Among the respondents, 41% of VA clinicians and 51% of ED clinicians reported instances of inadequate gel removal, which results in securement and dressing adherence issues. Poor adherence of dressings can lead to catheter failure and accidental dislodgement. Over half of all VA personnel (52%) said they felt that aseptic technique is often compromised by post-procedure gel clean-up.
PIV insertion is the most commonly performed invasive medical procedure among hospitalised patients. Over 70% of acute care patients require IV access at some point during their stay. According to Moureau, up to 60% of those patients may be considered to have difficult vascular access (DiVA). These patients frequently require ultrasound guidance in order to successfully achieve peripheral access and receive necessary treatments.
“This study confirms that the lack of consistent, evidence-based guidelines regarding ultrasound-guidance for PIV insertions has led to a great deal of fragmentation, and shows that clinicians are confused over when and how to use this technology in a way that protects patient safety,” said emergency vascular access expert Jon Bell (St Joseph Hospital, Bangor, USA). “There needs to be an objective standard for identifying difficult access patients, as well as a multidisciplinary effort to conduct research to determine the best practices that will minimise harm to the patient.”
The use of ultrasound may increase the risk of contamination during PIV insertions if certain guidelines are not followed to maintain a sterile insertion site and use the appropriate supplies (gel and transducer protection). According to Moureau, a specialty gel-free insertion dressing that separates the transducer and gel from the insertion site (UltraDrape, Parker Labs) may address and even mitigate many of these issues while reducing the cost of performing UGPIV insertions. In this study, 9% of survey respondents reported use of this gel separation safety dressing.
The survey results align with recent concerns from the healthcare quality and safety organisation, ECRI (Plymouth Meeting, PA). The non-profit technology assessment group addressed the issue of standardisation in its list of top patient safety concerns for 2020, writing that “policies and education must align across care settings to ensure patient safety.”
ECRI also included the use of point-of-care ultrasound in its briefing on 2020 Top 10 Health Technology Hazards, and noted that the rapid adoption of this technology across various care settings has left many organisations struggling to keep up with appropriate safety measures.













