
A tunneled catheter remains the most common access in patients initiating haemodialysis.1 This is most likely because the catheters are ready to use immediately after insertion, with no maturation time needed. As with any other dialysis access, hydraulic performance is critical for tunneled catheters. This depends mainly on the exit site, the shape of the catheter curve, and the tip position. In this report, Mohamed A Sheta and John R Ross discuss one important technical issue: the catheter tip.
In 2006, the Kidney Disease Outcomes Quality Initiative recommended that “at the time of placement, the tip(s) of the catheter should be in the mid-atrium, with the arterial lumen facing the mediastinum.”2 In one study, Mandolfo et al reported better blood flow with the catheter tip in the right atrium.3 In another study by McCarthy, the mean survival of catheters in the right atrium was 245 days, but only 116 days for catheters placed at the junction of the superior vena cava and the right atrium.4 Placing the tunneled catheter in the superior vena cava is related to early failure and low blood flow, perhaps due to direct suction force and the Bernoulli effect.
The most feared complications of the catheter tip being in the right atrium are dysfunction, infection, thrombosis, perforation, and cardiac arrhythmia. Engstrom et al studied the impact of laterality and tip position on catheter-related dysfunction and infection rate. Left-sided catheters terminating in the superior vena cava or pericavoatrial junction had significantly more episodes of catheter dysfunction or infection than catheters terminating in the mid- to deep right atrium. This effect was not seen in right-sided catheters.5 Also, evidence that low-lying catheter tips in the right atrium have higher perforation rates is lacking.6 Cardiac arrhythmia is a rare occurrence, and most of the cases relate to the guidewire rather that to the catheter tip itself.7
It is also critical to remember that dialysis catheters are inserted in the supine position but are used while the patient is in the sitting position, with a subsequent change in the position of the catheter tip relative to the right atrium. This is because of the descent of both the abdominal organs and the anterior chest wall structures. When the abdominal organs descend, the mediastinal structures (including the central veins and the right atrium) lengthen, causing the catheter tip to be at a higher level. Similar changes happen when the anterior chest wall structures descend inferiorly while the catheter is sutured to the skin. These changes are more prominent in obese patients.7
Generally speaking, there are four types of catheter tips: split, step, side-by-side, and two-tip catheters. Each has advantages and disadvantages. There are few studies comparing the effect of the catheter tip on blood flow, catheter survival, and complications with conflicting results. This is probably due to the multiple shapes of the right atrium (Figure 1).
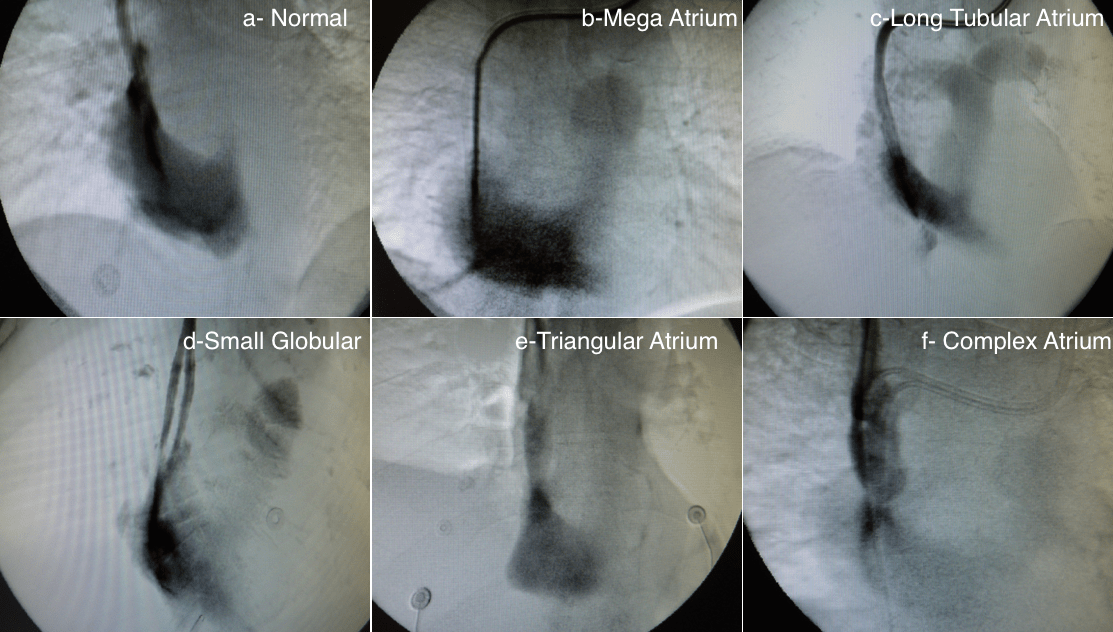
We strongly believe that each patient has their own “perfect catheter” and that one type should not be used for all patients. In our clinical experience, a split catheter is a good choice in normal and deep triangular atria. In a mega atrium, its globular shape will fit any type of catheter. In a long tubular atrium, a step-tip catheter is the best choice, while a side-by-side tip catheter will be more suitable for a small globular atrium. In a complex atrium, consider two-tip catheters. For these reasons, conducting a venogram to determine the shape of the atrium is a good practice.
Mohamed A Sheta and John R Ross, Regional Medical Center, Orangeburg, South Carolina, USA
References
- USRDS, chapter 4: Vascular access. https://www.usrds.org/2016/view/v2_04.aspx.
- National Kidney Foundation. Am J Kidney Dis 2006; Vascular access, CPG 2.4.
- Mandolfo S, Galli F, Costa S, et al. J Vasc Access Devices 2001; 2:106 –109.
- McCarthy M, Sadler D, Sirkis H, et al. AJR Am J Roentgenol 1999; 172:7.
- Engstrom B, Horvath J, Stewart J, et al. J Vascular and Int Radiology 2013;24:1295–1302.
- Rutherford JS, Merry AF, Occleshaw CJ. Anaesth Intensive Care 1994; 22:267–271.
- Vesely T. J Vascular and Int Radiology 2003; 14:527–534.













