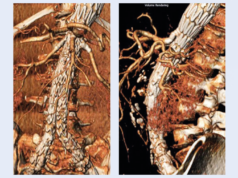
Twenty-four month TIGRIS trial follow-up data show that treatment using the Tigris nitinol stent (Gore) for long lesions in the superficial femoral and popliteal arteries is safe, effective and can “match stenting needs” in high-flexion areas with no reported stent fractures at 24 months despite a challenging patient population.
John Laird, University of California, Sacramento, USA, explained to delegates at the Vascular Interventional Advances 2016 (VIVA; 18–22 September, Las Vegas, USA), that there remains “an unmet need in the superficial femoral artery,” in combating “the complex forces at play and the potential for endoprostheses to undergo mechanical fatigue and fracture in this location”.
The Tigris is a dual component stent—the nitinol stent rings are coated with EPTFE and there is a fluoropolymer interconnecting structure incorporating a heparin bioactive surface. It is designed to conform to the anatomy and allow vessel movement, minimise fracture risk and allow axial compression while resisting stent elongation. The TIGRIS trial is investigating its effectiveness in treating de novo and restenotic atherosclerotic lesions of ≤24cm length in the superficial femoral and popliteal arteries of symptomatic peripheral artery disease patients. It is a prospective, multicentre, randomised, non-inferiority, control study, conducted at 33 sites in the USA and three in Europe, randomising 274 patients 3:1 to the Tigris stent and the Bard LifeStent (n=197 Tigris; n=70 LifeStent).
The two groups were well matched in baseline characteristics, and the majority had moderate or severe claudication. Three hundred and thirty-five Tigris stents were implanted in the 197 patients in that group, and 100 LifeStents were implanted in the 70 patients in the control arm. The lesions treated were long, with a pre-treatment mean lesion length of 107.6±68.6mm in the Tigris group and 117.9±75.4mm in the LifeStent group (p=0.292). The total stented length was 129±73.3mm in the Tigris group and 148.7±75.4mm in the LifeStent group (p=0.057).
The longest type of Tigris stent available for this study was 10cm, while the longest LifeStent allowed was 20cm long. Three stents were used in 36 (18.4%) of Tigris patients compared with four (5.7%) LifeStent patients. No LifeStent patients received four or more stents, while four patients (2%) in the Tigris group did. These patients had “a fairly high prevalence of total occlusions,” Laird said—83 patients (42.1%) in the Tigris group and 26 (37.1%) in the LifeStent group. Moderate to severe calcification was seen in 90 Tigris patients (47.6%) and 38 LifeStent patients (57.6%).
“Despite the complex nature of the lesions being treated, there was high device and lesion success, with no differences between the two groups with regards to the success rate,” Laird noted—99.5% device and lesion success in the Tigris group and 100% device and 97.1% lesion success in the LifeStent group. The primary safety endpoint—30-day freedom from major adverse events—was achieved in 99.5% of Tigris patients and all LifeStent patients. The primary efficacy endpoint—Kaplan-Meier estimated 360-day primary patency—was achieved in 63% of Tigris patients and 67% of LifeStent patients, a difference which was not statistically significant. This remained the case when estimating 24-month primary patency and freedom from target lesion revascularisation outcomes.
“One of the most interesting findings from the study was the very high fracture rate for the LifeStent,” Laird told the audience, with 17 (28.8%) fractures at 24 months. There were 10 complex fractures—five (29.4%) grade 4 fractures (misaligned stent fractures) and a further five (29.4%) grade 5 factures (transaxial spiral fractures). There were no fractures in the Tigris group. Laird also noted that both devices demonstrated minimal elongation (Tigris mean elongation of 0.03% and LifeStent mean elongation of 0.12%).
Patients in both groups showed a notable improvement in quality of life metrics. In the Tigris group, 87.9% of patients (n=145) saw an improvement in Rutherford classification, as did 89.7% (n=52) in the LifeStent group (p=0.71). Mean ankle brachial index improvement in the Tigris group was 0.25±0.23 versus 0.31±0.21 for the LifeStent group (p=0.53), mean EQ5D improvement was 0.1±0.2 for Tigris versus 0.13±0.2 for LifeStent (p=0.35) and mean Peripheral Artery Disease Questionnaire improvement was 29.84±24.09 for Tigris and 32.03±29.28 for LifeStent (p=0.57).
“Compared to previous superficial femoral artery investigational device exemption trials, this is clearly a more challenging and diseased patient population,” Laird said, “with the longest average lesion length and a great percentage of chronic total occlusions than most other trials.”