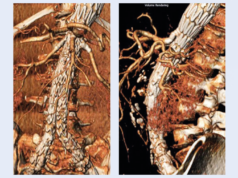
In patients with aortic dissection, a retrospective, population-based cohort study suggests that aortic branch involvement is responsible for “a significant long-term morbidity, without any related mortality”. This finding was recently published online in the Journal of Vascular Surgery (JVS).
Authors Francesco Squizzato (Mayo Clinic, Rochester, USA) and colleagues add that type B aortic dissection, patency of the aortic false lumen, or malperfusion syndrome at presentation had a higher risk of branch events during long-term follow-up. Furthermore, they write that dilatation of the aortic branches was observed in one-third of cases, in particular in the case of a patent aortic false lumen or Marfan syndrome.
Prior to their investigation, the authors note that late morbidity and mortality related to aortic branches in patients with aortic dissection were “not well described” in the literature. Therefore, it was their aim to investigate the fate of aortic branches in a cohort of patients with newly-diagnosed aortic dissection.
Using the Rochester Epidemiology Project record linkage system, the researchers identified all residents in Olmsted County, USA, diagnosed with aortic dissection from 1995 to 2015. They included only patients with >30 days of available follow-up imaging in the analysis.
Squizzato et al detail that the primary outcome of the study was freedom from any branch-related event (which the authors define as being any intervention, aneurysm, malperfusion, rupture, or death occurring after the acute phase >14 days) and that the secondary outcome was the diameter change of the aortic branches.
Of 77 total incident aortic dissection cases, the authors note that 58 patients who survived with imaging follow-up were included in the study—28 (48%) with type A and 30 (52%) with type B aortic dissection—and that the presentation was acute in 39 (67%) cases and six (10%) had branch malperfusion. Of 177 aortic branches involved by the aortic dissection, they add, 81 (46%) arose from the true lumen, 33 (19%) from the false lumen, and 63 (36%) from both.
Squizzato and colleagues also relay that, after the acute phase, freedom from any branch-related event at 15 years was 48% (95% confidence interval [CI], 32–70). In addition, they state that 31 branch-related events occurred in 19 patients over 15 years: 12 interventions (76% freedom; 95% CI, 63–92), 10 aneurysms (67% freedom; 95% CI, 50–90), eight malperfusions (76% freedom; 95% CI, 61–94) and one rupture (94% freedom; 95% CI, 84–100). There were no branch-related deaths, they report.
Writing in JVS, the authors further detail that type B aortic dissection (hazard ratio [HR], 3.5; 95% CI, 1.1–10.8; p=0.33), patency of the aortic false lumen (HR, 6.8; 95% CI, 1.1–42.2; p=0.038) and malperfusion syndrome at presentation (HR, 6; 95% CI, 1.3–28.6; p=0.023) were predictors of late aortic branch-related events.
Squizzato et al acknowledge some limitations of the present study, including its retrospective nature, which may have led to “inherent biases” due specifically to the initial code-based identification of patients with aortic dissection. Also, they recognise that the limited number of patients included in the final cohort “may have limited the power of the statistical analysis”. In particular, they write that it was not possible to discriminate the effect of complete versus partial thrombosis of the aortic false lumen on branch-related complications.
Despite these drawbacks, the authors also highlight a number of key strengths to their study. They explain that the population-based approach, for example, allowed them to gather detailed follow-up information and to report reliable long-term follow-up results, since their patient cohort was not subject to the referral bias usually noted in registry or single-centre reports.
In addition, they communicate that they tried to include in the primary endpoint only clinically significant events, excluding sub-aneurysmal arterial dilatations and imaging findings that were not associated with any clinical or laboratory manifestations.
Summarising the overall importance of their study, Squizzato and colleagues write: “The findings of statistically significant results in a relatively small sample size suggests that these factors truly have a clinically significant impact on the population of patients affected by aortic dissection.”