A mid-term assessment of bridging stentgraft integrity and flare geometry following fenestrated endovascular aortic repair (FEVAR) finds that, although there is a substantial reintervention rate post-procedurally, most are not related to the use of balloon-expandable covered stents (BECS). This is the conclusion presented by Jean Paul de Vries (Groningen, The Netherlands) at the 2021 Charing Cross Symposium (CX; 19–22 April, online) yesterday. He informed his audience that computed tomography (CT)-applied software enables the visualisation of precise BECS-morphology, allowing interventionalists to see changes during follow-up. “These changes in flare geometry and D-ratio may predict later failure,” he explained.
“FEVAR has been associated with a high technical success rate, low-intra-operative visceral artery occlusion rate, and a low 30-day mortality rate,” de Vries told attendees during the “Juxtarenal controversies solved” session. However, there is a substantial reintervention rate at mid-term [three- to five-year] follow-up of 27–42%. BECS-associated complications can be endoleaks, obstructions, and fractures.”
According to the speaker, the current FEVAR literature focuses primarily on the short-term outcomes of the procedure, and contemporary diagnostic modalities centre on complications instead of on predicting or preventing complications. Furthermore, de Vries said there is presently a lack in ability to precisely determine BECS morphology during follow-up.
The investigators of the BUTTERFLY study therefore looked at the mid-term outcomes of the bridging Advanta v12 BECS (Getinge) after FEVAR. They used dedicated software to determine stent morphology and possible modes of failure during follow-up.
In total, 194 consecutive FEVAR patients treated between 2012 and 2015 at either the General Hospital Nuremberg (Nuremberg, Germany) or UMCG Groningen (Groningen, The Netherlands) were enrolled in the study. Patients were treated with a primary FEVAR (177) or fenestrated cuff (17), and at least one of the fenestrations had to be bridged by the Advanta V12.
Patient survival was 68% at five-years follow-up.
Turning to reintervention rates, de Vries commented: “Freedom from reintervention drops to 60% at five-year follow-up.” Reintervention was largely necessary due to a type I or type II endoleak. Three patients had a rupture requiring reintervention post-FEVAR, four patients needed reintervention for a BECS-related complication (stenosis or occlusion), and other reinterventions were indicated due to iliac artery access complications or bleeding.
“Freedom from BECS-related complications is high at five-years, at 98%” he continued. Focusing on the patients who experienced BECS-related complications (stenosis, occlusion or type IIIc endoleak) late in follow-up, de Vries noted: “Only five patients had a BECS fracture, three without any complication, one with a stenosis, and one with an occlusion.
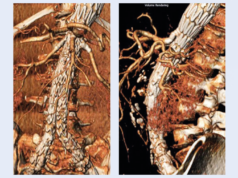
“We used a homemade CT-applied software to calculate the exact morphology of the flare part of the balloon-expandable covered stent. We could measure the flare to fabric distance, and also the D-ratio.”
Giving an example of the software in action, he detailed how a right renal balloon-expandable covered stent migrated in one patient included in the study, and showed 3D images of how he and his team could visualise and trace this movement out to two-years. In another illustration of the software’s utility, he discussed a patient who had a circular flare at 42-days follow-up; at two-years, there was compression of this flare. While this was not noticed during the CT scan, de Vries told CX attendees: “It was not noticed during the CT scan, but with the applied software, we can calculate it and make it visible, and can reintervene.”
While he concluded that there is still a substantial reintervention rate post-FEVAR, he emphasised that most reinterventions are not BECS-related, and enthused about the role of CT-applied software in predicting later failure, facilitating timely reintervention.