This advertorial is sponsored by Philips.

Two early adopters of Fiber Optic RealShape (FORS; Philips) share their expert opinions on the developing technology, highlighting its future potential in reducing radiation and increasing procedural efficiency.
The European Society for Vascular Surgery (ESVS) 2023 clinical practice guidelines on radiation safety1—the first recommendations on the topic to be published in the vascular surgery domain—brought into sharp focus the need to address radiation exposure during endovascular aortic procedures.
Bijan Modarai (Guy’s and St Thomas’ NHS Foundation Trust and King’s College London, London, UK), lead author of the guidelines, notes that X-ray-guided endovascular procedures have become the “mainstay” treatment modality for patients with vascular disease. X-ray is the current standard of care for endovascular procedures, he says. However, it has drawbacks, and the associated radiation poses a threat to patients and operators alike. Based on extensive research into radiation-induced DNA damage, Modarai and colleagues at King’s College London have identified biological evidence that radiation is having a negative effect on both patients’ and operators’ cells.
Adding to the problem are two factors, Modarai says, noting that practitioners are nowadays being exposed to X-rays throughout their entire career, and that the increasing complexity and thus length of endovascular procedures is resulting in “significant” radiation exposure to both the patient and, “crucially,” the operator.1
The ESVS guidelines aim to raise awareness of the risks of radiation and provide guidance on best practice, closing with a forward-looking chapter on the importance of new and future technologies in reducing and, in the longer term, eradicating the need for radiation. Fibre optic guidance is one such technology, with reference made not only to its radiation-reducing potential, but also to how it might enhance visualisation of catheters and wires and lead to potentially shorter procedure times.1,2
Joost van Herwaarden (University Medical Center Utrecht, Utrecht, The Netherlands), who led the first-in-human clinical feasibility study of endovascular navigation with FORS,3 notes that mention of the technology in the guidelines is important for the purpose of generating awareness and interest among the vascular community. “All of us should be aware that there are other possibilities than just using fluoroscopy,” he comments.
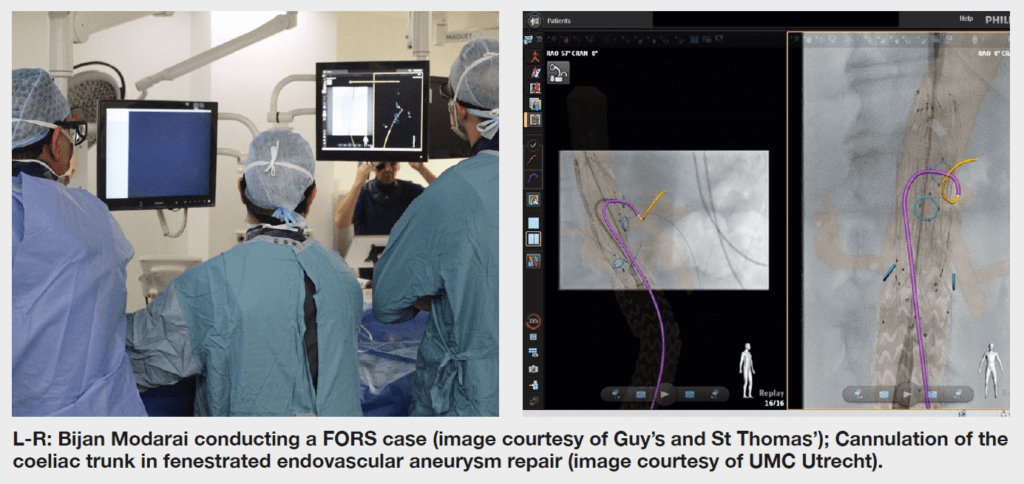 Modarai, who recently performed the first fibre optic-guided case at Guy’s and Thomas’ NHS Foundation Trust, concurs, stating that increasing interest in developing technologies to address the radiation issue “has to be high on the list of priorities for all stakeholders”.
Modarai, who recently performed the first fibre optic-guided case at Guy’s and Thomas’ NHS Foundation Trust, concurs, stating that increasing interest in developing technologies to address the radiation issue “has to be high on the list of priorities for all stakeholders”.
“We wanted to disseminate knowledge about what is currently in the pipeline, with the hope that that will stimulate interest in those who read [the guidelines] to come up with new research endeavours,” Modarai explains.
A “novel way” to visualise and navigate the aorta
Van Herwaarden states that he and two other operators have now performed a combined total of around 150 cases with FORS at the University Medical Center Utrecht. “We are getting used to it,” he says, noting that the team have seen improvements with the technology in the three years since they started using it. He mentions that with the recent introduction of Philips’ 3D Hub technology, for example, it is possible to use many different commercially available catheters and show them with the FORS technology. The team now use FORS weekly and in “almost all endovascular aneurysm repairs,” van Herwaarden details. Specifically, he tells Vascular News that FORS “really gives you a better understanding of the position and 3D morphology of the devices in the 3D anatomy or workspace,” noting that the better view the technology provides makes cannulations easier.
For Modarai, fibre optic technology represents a positive addition to his aortic practice. “The fact that you can visualise the catheter and the wire relying on this technology rather than X-ray is a conceptual advance,” he says. The benefits of the technology, in Modarai’s view, are multifactorial, pointing to its potential to protect both the patient and the operator from radiation, whilst also providing a “novel way” to visualise and navigate the aorta. “You get a view of the area that you are navigating in multiple planes,” he explains, “and that in itself also facilitates the procedure, allowing the entire team in the hybrid operating theatre to be able to follow what is going on and to be able to visualise what is being done on the screen”.
With regard to the literature on FORS, the evidence base is growing. Most recently, Eric J Finnesgard (University of Massachusetts Chan Medical School, Worcester, USA) and colleagues, under the senior authorship of Andres Schanzer, outlined an initial single-centre experience using FORS guidance in complex endovascular aortic repair. In November 2022, they reported online in the Journal of Vascular Surgery that FORS has shown “promise” in their aortic practice, with “acceptable technical success and reductions in procedural times and radiation usage”.2 Schanzer is set to share these findings, as well as his experience so far using FORS, at the Charing Cross (CX) Symposium 2023 (25–27 April, London, UK).
Van Herwaarden believes that FORS will have positive effects on radiation. He stresses, however, that this still has to be proven, which is why he and his team together with seven other renowned centres in Europe and the USA are conducting a registry study. “We are now busy with the analysis of the more than 600 cases that have been done,” he explains.
While data are being collected, van Herwaarden is keen to stress that FORS is still in its early stages. “It feels like we are still in the beginning of a new technology that is slowly proving itself,” he remarks, and is looking ahead to a “promising” future where FORS could enable less need for radiation, quicker procedures, and fewer complications.
According to van Herwaarden, the future of FORS lies also in its combined use with other emerging technologies, for instance robotic tracking, artificial intelligence, and intravascular ultrasound (IVUS), with the combination offering “an even greater promise for simplifying complex procedures and realising radiation dose reduction for patients and for staff”.
Modarai believes the technology will be “transformative” in endovascular aortic procedures, while adding the caveat that there is still some way to go. He looks ahead to iterative improvements with regard to compatible wires and catheters, and the footprint of the ancillary devices, for example, which will make fibre optics “easier and easier” to incorporate into clinical practice. Eventually, he hopes, it will become an “essential” part of the workflow, allowing operators to circumvent the use of X-rays for endovascular procedures. “When that goal is reached, then it is difficult to imagine that one would want to perform these procedures without a technology like this.”
References
- Modarai B, Haulon S, Ainsbury A, et al. Editor’s Choice – European Society for Vascular Surgery (ESVS) 2023 clinical practice guidelines on radiation safety. European Journal of Vascular and Endovascular Surgery. 2023;62(2):171–222.
- Finnesgard EJ, Simons JP, Jones DW, et al. Initial single-center experience using Fiber Optic RealShape guidance in complex endovascular aortic repair. Journal of Vascular Surgery. Published online first 12 November 2022.
- Van Herwaarden J, Jansen MM, Vonken EPA, et al. First in human clinical feasibility study of endovascular navigation with Fiber Optic RealShape (FORS) technology. European Journal of Vascular and Endovascular Surgery. 2021;61(2):317–325.