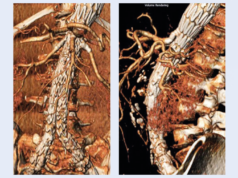
At the 2017 Vascular Annual Meeting (VAM; 30 May–3 June, San Diego, USA), mid-term follow-up data from a pivotal trial (IBE 12-04) of the Excluder Iliac Branch Endoprosthesis (IBE, Gore) and the real-world GREAT Registry showed that the device is effective at treating common iliac artery and aortoiliac aneurysms, maintaining blood flow into the internal iliac artery, and avoiding complications associated with internal iliac artery sacrifice.
The Excluder device has been designed to preserve internal iliac artery perfusion during endovascular repair of aortoiliac aneurysms and common iliac artery aneurysms. Darren B Schneider (New York, USA) told VAM delegates, “Common iliac artery aneurysms are present in approximately 25% of patients undergoing endovascular aneurysm repair (EVAR),” Schneider told delegates. The goal of iliac branch devices is to allow treatment of these aneurysms while preserving hypogastric artery patency. Schneider noted that the vital measures of success for these devices are technical success >90%, low morbidity and mortality, primary patency rates of 75–100% and prevention of pelvic ischaemic complications (such as buttock claudication).
Previously-published six-month data of 63 patients from the IBE 12-04 trial reported mean common iliac aneurysm side on the IBE side of 41±11.4mm (range 25.2–76.3mm). There were no procedural deaths and technical success was 95.2% (n=60/63). Internal iliac limb patency was 95.2% (n=60/63), and no new type I or III endoleaks or device migrations were observed at six months. The three patients with loss of internal iliac limb patency were asymptomatic, and freedom from new-onset buttock claudication on the IBE side was 100% at six months. New-onset buttock claudication occurred on the non-IBE treatment side in six of 21 patients (28.6%) who underwent staged internal iliac artery coil embolisation. The freedom from reintervention rate was 98.4%.
At VAM, Schneider presented “extended” IBE 12-04 follow-up data for 98 patients (98.9% male, age 69±9.3 years, and with maximum iliac diameter 39.3±10.9mm) at a mean follow-up of 650 days. He noted that there was no off-label use of the device in this cohort. Percutaneous access was performed in 55.1% (n=54) of patients and cut down access in 40.8% (n=40). Procedural survival was reported in all 98 patients.
The data from the GREAT Registry were from 92 patients (92.4% male, age 72.7±7.7 years, and with maximum iliac diameter 36.6±11mm) at a mean follow-up of 315 days. Contrasting to the IBE 12-04 trial, this real-world Registry had 57 (62%) cases of off-label device use. Percutaneous access was used in 40.2% (n=37) of patients and cut-down access in 48.9% (n=45). As in the IBE 12-04 trial, procedural survival was 100%.
In the IBE 12-04 trial cohort, there was no aneurysm-related mortality. Seven (7.1%) cases of all-cause mortality were reported, along with eight (8.2%) reinterventions. Eight iliac occlusions (8.2%) were observed, and there were no cases of new onset ipsilateral buttock claudication.
There was also no aneurysm-related mortality in the GREAT Registry patients. There were seven six (6.5%) all-cause mortalities and six (6.5%) reinterventions. Of the 49 iliac arteries treated there were six (9.4%) occlusions and there were no new onset ipsilateral buttock claudications.
There were no reported type III endoleaks in either the IBE 12-04 trial or the GREAT Registry. There were three (3.3%) type I endoleaks in the GREAT Registry (none in IBE 12-04), while there were two (2.2%) type II endoleaks in the GREAT Registry and seven (7.1%) in the IBE 12-04 trial.
“EVAR using the IBE device was effective with good mid-term outcomes in both the multicentre trial and real-world settings,” concluded Schneider. “Through three years of follow-up, freedom from complications, device occlusion and reintervention is excellent and support the use of iliac branch devices for treatment of common iliac artery aneurysms. Follow-up will be continued for five years to establish the long-term durability of iliac aneurysm repair with the IBE device.”