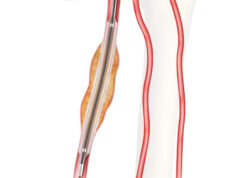
The Eluvia drug-eluting vascular stent system (Boston Scientific) shows superior primary patency compared to the Zilver PTX drug-eluting stent (Cook Medical), concludes the 12-month follow-up of the IMPERIAL randomised controlled trial. These data were presented for the first time at the Cardiovascular and Interventional Radiological Society of Europe (CIRSE) 2018 meeting (22–25 September, Lisbon, Portugal).
The data were also presented at the TCT conference and are accompanied by simultaneous publication in The Lancet.
The IMPERIAL trial was a prospective, randomised, single-blinded, multicentre global study aimed at comparing the effectiveness and safety of the Eluvia with Zilver PTX for treatment of symptomatic femoropopliteal artery lesions (lesion length 30–140mm, Rutherford category 2–4).
Presenting the results, Stefan Müller-Hülsbeck (Flensburg, Germany; the European primary investigator) told the CIRSE audience: “Clinical outcome rates were similar between groups, but with half the revascularisation rate for Eluvia.” For instance, the Eluvia stent had a target lesion revascularisation rate of 4.5%, in contrast to 9% observed within the Zilver PTX cohort.
Additionally, the Eluvia stent was found to be more effective than the Zilver PTX, with a primary vessel patency of 88.5% at 12-months versus 79.5% after the same time-frame. Primary vessel patency is defined as a core lab-assessed duplex ultrasound peak systolic velocity ratio of ≤2.4 in the absence of clinically-driven target lesion revascularisation or bypass of the target lesion.
Both the Eluvia stent system and the Zilver PTX—which are designed to restore blood flow in the superficial femoral and proximal popliteal arteries—feature a drug-polymer combination intended to allow for the sustained release of paclitaxel. This drug can prevent restenosis of the vessel.
However, the presence of a polymer (a biostable fluorinated polymer matrix) contained within the Eluvia stent allows for a lower dose of paclitaxel, which is indicative of the main difference between the two stents.
Speaking to the CIRSE audience about the reasons for the findings, Müller-Hülsbeck alluded to the presence of the polymer being the “key to success”.
“These impressive clinical outcomes suggest that sustained elution of paclitaxel, delivered by the Eluvia stent, better matched the timing of restenosis in the SFA that can occur months later, thereby reducing the need for repeat interventions,” said William Gray, co-principal investigator of the IMPERIAL trial. “Based on these findings, we believe that the Eluvia stent can be a preferred therapy option when treating patients with arterial blockages in the superficial femoral or proximal popliteal arteries.”
Off the back of data from the MAJESTIC trial, which evidenced long-term freedom from revascularisation at three years, the Eluvia stent system received the CE mark in early 2016. With a primary patency rate of more than 96%, the MAJESTIC trial results represented the highest 12-month primary patency reported for an interventional treatment of femoropopliteal artery lesions among comparable trials, according to Boston Scientific.
The Zilver PTX drug-eluting stent also has a wealth of strong clinical data supporting its efficacy. In 2009, the device was the first CE mark-approved drug-eluting stent designed specifically to treat severe blockages in the superficial femoral artery. Five-years results from the largest and longest-running clinical trial of a drug-eluting stent for treating peripheral arterial disease, published in 2014, evidenced long-term patency for patients treated with the Zilver PTX. This 2014 study compared the Zilver PTX with a bare metal stent, and confirmed the “sustained benefit” of the paclitaxel-eluting stent.