There was consensus on day one of the CX Aortic Vienna 2022 Digital Edition (24–26 October) that aortic sac regression is a positive sign and that, following endovascular aneurysm repair (EVAR), it is important to monitor any sac increase and investigate its cause. In answer to a polling question in a session on abdominal aortic pathologies, 93% of attendees voted that “sac diameter increase is an indicator of endoleak somewhere”.
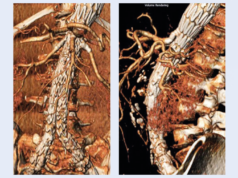
This decisive polling result followed a presentation by Daniela Branzan (Leipzig, Germany) on aortic aneurysm sac regression following pre-emptive embolisation of aneurysm sac side branches for endovascular aneurysm repair (EVAR). Branzan concluded that embolisation of aneurysm sac side branches in patients with abdominal aortic aneurysm (AAA) is “safe and effective in preventing type 2 endoleak for EVAR”.
The presenter reported having observed shrinkage of the aneurysm sac in a high proportion of patients with pre-emptive embolisation of aneurysm sac side branches. However, she also noted that definitive evidence for routine embolisation of aneurysm sac side branches to prevent type 2 endoleak after EVAR and promote shrinkage of the AAA sac requires a randomised controlled trial. Moderator Alexander Zimmermann (Zurich, Switzerland) remarked that this is perhaps the “hottest topic” in the area of EVAR.
In this session, anchor Roger Greenhalgh (London, United Kingdom) was joined by moderators Zimmermann, representing the Swiss Society for Vascular Surgery (SGG), and Markus Steinbauer (Regensburg, Germany), who is the current president of the German Society of Vascular Surgery (DGG). The session was designed to bring some of the discussion points from two dedicated CX Aortic Vienna sessions at last week’s Dreiländertagung (19–22 October, Vienna, Austria) to a global audience.
The moderators represented two of the three societies that make up the Dreiländertagung, with one of the speakers in this session—Afshin Assadian (Vienna, Austria)—representing the third society involved: the Austrian Society of Vascular Surgery (OGG). Assadian spoke on established and rare indications for endovascular repair in the very young, concluding that a growing population of very young patients needs aortic repair for dilative pathologies. He recommended that individual case planning with a clear view for future conversion of EVAR into open repair or fenestrated EVAR (FEVAR) is important and justifies offering endovascular therapies in this population. Greenhalgh pointed out the importance of industry creating devices that change with the growth of the aorta in this field.
Steinbauer also spoke in this session, addressing the endovascular treatment of type 1 endoleaks with inner branched devices. He concluded that endovascular repair of a type 1a endoleak is feasible, noting however that the planning and implementation are “complex” and that the technique comes with specific risks and technical challenges. He said that his first choice of treatment is fenestration, however noted that certain anatomical challenges—for example a narrow aorta or kink—make it impossible to open up a fenestrated graft. In cases such as this, he would use inner branched devices.
Another speaker in this session was Vladimir Makaloski (Bern, Switzerland), who gave a presentation on physician-modified endografts at the visceral and iliac levels. He concluded that these devices are helpful in urgent and emergency cases, as there is no delay with treatment, and also highlighted the lower costs compared with custom-made alternatives. Makaloski added that surgical modification can be used in all anatomies, warning however that these devices are outside the instructions for use (IFU). “There is a learning curve,” he said, closing his presentation.