The first session of CX Aortic Vienna (8–11 September, virtual) saw expert speakers discuss different approaches to abdominal aortic aneurysm repair—including open and endovascular techniques. Gustavo Oderich (Houston, USA) opened the session detailing an experimental ex vivo endovascular aneurysm repair (EVAR) using Centerline Biomedical’s IntraOperative Positioning System (IOPS)—an electromagnetic image guidance technology—without fluoroscopy.
This session, and all other sessions from day one of CX Aortic Vienna, is available to view on demand. Click here to register and access the recording.
“We are all aware of the deleterious effects of ionising radiation-especially when dealing with complex endovascular aortic repair, which carries on average 3–15 times higher radiation exposure,” he told the audience, before detailing the use of the IOPS system in a test case using a 3D printed model. “I believe this represents a first step towards allowing these procedures to be done without radiation, and finally getting rid of our infamous lead apron,” he commented.
Majority of CX audience agree hospitals should provide uninterrupted access to EVAR for rAAA
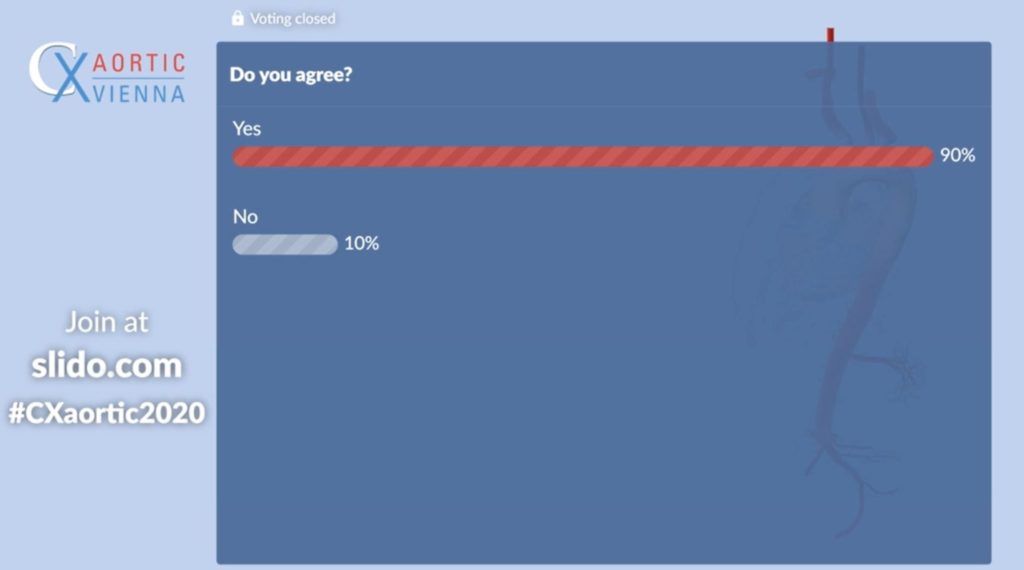
In the following presentation, Thomas Forbes (Toronto, Canada) argued that, ideally, hospitals should provide uninterrupted access to endovascular repair for ruptured abdominal aortic aneurysm (rAAA), or not at all. “The uptake of endovascular repair of rAAA has resulted in fewer instances in no repair and reduced turn down rates,” he noted, and in polling following Forbes’ presentation, it was revealed that 90% of the audience agreed with the statement “Hospitals should provide uninterrupted access to endovascular repair for rAAA”.
To illustrate current techniques, Jean Panneton (Norfolk, USA) presented a case study of a 65-year-old male patient, presented with a ruptured juxtarenal AAA. He also outlined the key principles that need to be in place for a ruptured AAA programme, detailed the requirements for a rEVAR-ready hospital and discussed aortic balloon occlusion sequencing utilising a double sheath technique. According to Panneton, establishing an aortic alert and implementing a ruptured AAA protocol are essential to improve outcomes.
“Acute and early conversions are really rare in modern EVAR,” said Michel Makaroun (Pittsburgh, USA), whose presentation covered the topic of open conversion following failed EVAR, which he said, is still required in many cases. Makaroun detailed that frustration with ineffective endovascular solutions is driving an increase in utilisation of open conversion, which he noted carries a higher mortality and morbidity than de novo repair, mostly in patients with ruptures or infection. “Explantation is not required in all cases,” he remarked, adding that “limited interventions are effective, safe, and may reduce mortality and morbidity of conversions”.
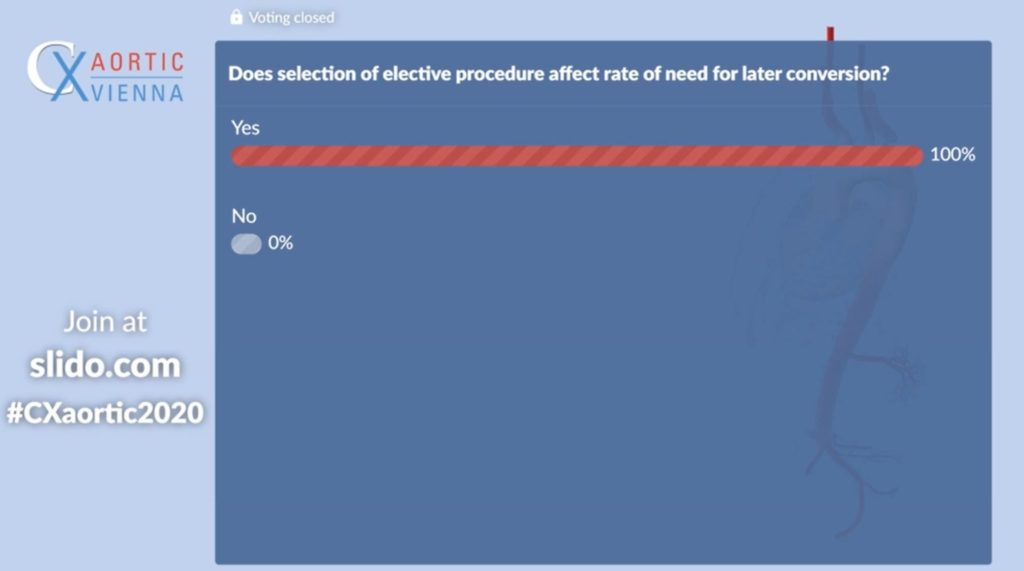
Polling finds 100% of audience believe selection of elective procedure affects the rate of need for later conversion
During his presentation, Frank Vermassen (Ghent, Belgium) detailed semi-conversion, which he described as: “A less well known technique in the treatment of growing aneurysms after EVAR”. Semi-conversion is an alternative technique to embolisation or open repair, and sees an aneurysm exposed through a transabdominal or retroperitoneal approach, involving banding of the proximal neck, followed by incision of the aneurysmal sac, removal of the thrombus and closure of the sac. Semi conversion offers “clear advantages”, Vermassen said, especially in frail patients due to its less invasive approach and is an “interesting third way in the treatment of growing aneursysms after EVAR”.
Following Vermassen’s presentation, the audience were asked if the selection of an elective procedure affects the rate of need for later conversion, to which 100% of voters responded in the affirmative.
Incidence of late conversion after EVAR has risen in recent years, according to Daniele Mascia (Milan, Italy), due to the growing rate of EVAR procedures since the turn of the century. He presented 15-year experience of EVAR conversion from 84 cases, 81 of which involved endograft removal. Mascia commented that late conversions after EVAR represent a technical challenge, but can achieve better results in high volume aortic centres and highlighted the need for close follow-up, especially in young patients.













