This advertorial is sponsored by Bentley.

Based on his high-volume experience of branched repairs, Said Abisi, consultant vascular and endovascular surgeon at Guy’s and St Thomas’ NHS Foundation Trust (London, UK) offers his expert opinion on the use of the BeGraft PLUS (Bentley InnoMed GmbH) in thoracoabdominal aortic aneurysms (TAAAs) treated with branched endografts (BEVAR). Speaking to Vascular News, Abisi outlines the challenges of bridging stents in branched procedures, some crucial and desired features of a bridging stent, and why the BeGraft PLUS is the stent of choice in TAAA anatomy.
New, multicentre data support Abisi’s claims. At LINC 2021 (The Leipzig Interventional Course; 25–29 January, online), Abisi presented data on branched cases that he has evaluated together with Eric Verhoeven (General Hospital Nuremberg, Paracelsus Medical University, Nuremberg, Germany), showing “very promising” patency rates overall.
In your experience, what are the key factors behind a successful BEVAR procedure?
I have been performing branched procedures at a relatively high volume for just over seven years now. A successful BEVAR procedure is a multifactorial process and is heavily dependent on a bridging stent. Over the years, we have evolved and changed our practice with regard to the devices we have used. In the past, self-expanding covered stents were used most often, but there were certain challenges related to their deployment, precision, and radial force. We often had to reline these stents and do various adjunct procedures to avoid compression, occlusions, and/or kinks, as well as to prevent migration and endoleaks.
Three years ago, I changed my practice to using balloon-expandable covered stents because of these problems. I have been using the BeGraft PLUS ever since. We are very satisfied with the performance of this stent for various reasons, including precision, visibility, ease of deployment and—most importantly— outcome. In our practice with the BeGraft PLUS, we have seen both a low occlusion rate and a low reintervention rate.
In your opinion, what are the main features that a bridging stent needs to have?
First of all, I believe there is no “fit all” solution for bridging stents. Bridging stents for fenestrated procedures do require different features compared to branched procedures. In general, however, there are a number of key features that a bridging stent needs to have in both fenestrated and branched procedures. Firstly, it needs to be flexible. Cobalt chromium is the metal used in these stents. It is flexible but also ensures that the stent can maintain radial force, which is maximised because of the unique structure of two layers. Another key feature is precise deployment. In a branched aortic procedure, we often use an access point that is far from the implantation site, for example upper limb or retrograde, and so we cannot afford any lack of accuracy during stent placement. Therefore, it is highly important to navigate safely with reliable deployment and superior visibility.
We continue to identify challenges associated with selecting a bridging stent in branched repair. Many of us are concerned about the length of covered stents and how far within the target vessels they have to be placed to maintain a good position and prevent endoleaks. A good bridging stent for branched procedures must have adequate radial force in order to meet this need, without excessively extending into the target vessel. We are happy that the radial force of the BeGraft PLUS seems to maintain excellent seal at 15mm within renal arteries and 20mm in larger target vessels, such as the superior mesenteric and coeliac arteries. Since starting to use the BeGraft PLUS, we have not seen any branch-related endoleaks.
One of the things we would like from a future bridging stent would be for it to be able to go far enough into the vessel, but for it not to be very intrusive distally where target vessels movements can be greater.
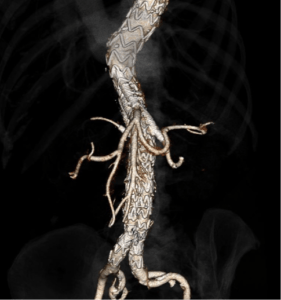
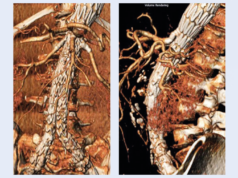
branched procedure
Besides the commonly-known outer branched stent graft designs, there is a new trend of stenting the inner branches in TAAA procedures. What are the major differences between inner branches and outer branches, and are there additional challenges for bridging stents when you use them in inner branches?
One of the main differences is the distance between branch and target vessel. Generally speaking, you will need a shorter bridging stent for an inner branch than you will for an outer branch because of the proximity between the inner branch and the target vessel. Additionally, there is a shorter distance to bridge between the inner branch outlet and the target vessel ostium, and so, theoretically, there should be less stress on the bridging stent or risk of compression.
Other than that, I have not seen any significant differences between outer and inner branches or challenges associated with inner branches from a bridging stent point of view. On the contrary, one of the advantages I have seen for the inner branch is that, once the bridging stent is in the branch, tracking it into the target vessel seems to be more stable, which is possibly due to the fact that the inner branch is stabilised inside the main graft and provides a solid platform from which to advance the bridging stent. However, it is difficult to make a direct comparison because we are treating different pathologies with the two types of branches.
Would you use different covered devices in inner and outer branches?
No, I would use the same stent in both inner and outer branches because it has worked well in our practice so far. The Journal of Endovascular Therapy recently published some of our data on covered stent use in both inner and outer branches,1 and these showed that that there was no difference in performance between the two.
You presented some data on these procedures at LINC 2021. What were your key findings from the branched cases that you have evaluated together with Eric Verhoeven?
At LINC 2021, we presented multicentre data from London and Nuremberg looking at BeGraft PLUS performance in both inner and outer branches from two high-volume users. We have seen a very promising patency rate of 98.6% so far and we have not encountered any significant primary technical issues. In the London series, we had a significant number of patients who had inner branches, and these all had excellent outcomes.2
We also considered the rates of stent relining and extension. Thanks to the stent resistance feature of the BeGraft PLUS, relining is required less frequently compared to other self-expanding or balloon-expandable bridging stents. We never primarily reline a BeGraft PLUS because we do not see the need from it. Published data from London show a 3% rate of relining to smooth the distal transition zone with a self-expanding stent in the target vessels. In fact, longer follow-up of patients treated in London confirmed 98% patency without primary relining at 18-month follow-up. We do extend with an additional bridging stent if we need to, for example if we feel the distal sealing zone is incomplete or needs to be optimised. Overall, our extension rate is 21% in our recently-published data from London.
References
- Abisi S, Gkoutzios P, Carmichael M, et al. The early outcomes of BeGraft Peripheral Plus in branched endovascular repair of thoracoabdominal aneurysms. Journal of Endovascular Therapy 2021. Article in press.
- Abisi S, Zymvragoudakis V, Gkoutzios P, et al. Early outcomes of Jotec inner-branched endografts in complex endovascular aortic aneurysm repair. Journal of Vascular Surgery 2021. Article in press.