The first patient has been treated with NeuroFlo perfusion augmentation technology (developed by CoAxia Inc.) in a feasibility study to assess its effectiveness in patients who do not respond to thrombolysis with the drug tissue plasminogen activator (tPA), the only stroke therapy currently approved by the FDA. The technology is already being evaluated as a stand alone treatment for patients that are outside the three hour tPA treatment window.
The procedure was performed on a 35 year old stroke victim whose symptoms and cerebral imaging showed no improvement following administration of tPA. Following NeuroFlo treatment, the patient had a significant improvement in blood flow to the brain and in motor and speech function, with no adverse events. Co-principal investigators, Drs Ken Butcher, Derek Emery and Ashfaq Shuaib are leading this 20 patient feasibility study to investigate the safety of using cerebral perfusion augmentation in patients who receive tPA but do not respond clinically. While thrombolysis is the only stroke treatment proven safe and effective in a randomized trial, only a minority of patients benefit from a near complete recovery. There remains significant need for adjunctive treatments in this important patient group.
Shuaib, Director of Stroke Services at the University of Alberta commented, “CoAxia is already conducting studies to demonstrate that NeuroFlo treatment may be effective as a stand alone treatment, and we are excited to extend this work to patients who do not respond to pharmaceutical interventions. This feasibility study is an important step to show that NeuroFlo treatment is a good adjunct to tPA therapy.”
The CoAxia technology is a potential alternative or complement to these clot-focused techniques. The brain has an extensive, interconnected collateral vascular network. Already somewhat active following an ischemic stroke, collateral pathways are capable of further increasing the delivery of oxygenated blood to the stroke’s ischemic penumbra. The ability to salvage that penumbra and minimize the eventual size of the infarct may lead to improved neurological recovery.
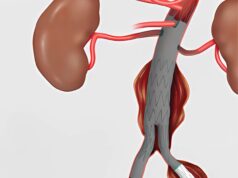
The NeuroFlo catheter augments the blood flow to the brain and in particular increases blood flow in the collateral blood vessels to augment perfusion in the ischemic penumbra. NeuroFlo partially restricts blood flow in the descending aorta, diverting blood flow from the lower extremities to the cerebral collaterals. The NeuroFlo catheter itself is a unique, dual-balloon endovascular device. It is inserted through the femoral artery into the descending aorta and has independently inflatable balloons located immediately above and below the renal arteries. The balloons are sequentially inflated to produce occlusions of approximately 70%. The balloons are left inflated for 45 minutes and are then removed and treatment is complete.
In addition, since the therapy does not attempt to remove or disturb the clot, it may be less likely to cause hemorrhage, a common complication of other acute stroke treatments. NeuroFlo has been evaluated up to 12 hours beyond onset and could become a viable treatment alternative for the hundreds of thousands of patients that are too late to treat with current options.
This concept was first tested through animal experimentation, which demonstrated that partial aortic occlusion could be accomplished without significant side effects, cerebral perfusion could be rapidly and significantly increased, and the size of a resulting infarct could be reduced. In April 2002, the first clinical studies began in humans to demonstrate the safety of the procedure. In 29 stroke patients treated during CoAxia’s feasibility studies 61% of patients improved by more than three NIHSS points during the NeuroFlo procedure and 62% had an improvement of three NIHSS points at 24 hours. The significance of this improvement is reinforced by the fact that the average time to treatment in these patients was 7.5 hours after the symptom onset, well beyond the three hour treatment window of the FDA-approved intravenous tPA. These feasibility results provided the basis for CoAxia’s current SENTIS pivotal trial, and its recent SafeFlo24 feasibility study.
0-10 hour strokes
In addition to this feasibility study, CoAxia has two additional stroke studies underway, the SENTIS randomized pivotal trial of patients up to ten hours after stroke onset, and the Flo24 safety and feasibility study of patients as late as 24 hours after stroke. SENTIS (Safety and Efficacy of NeuroFlo Technology in Ischemic Stroke) is being conducted at leading stroke centers in North America. The trial will determine if this unique method for increasing blood flow to the brain (with a catheter partially occluding the aorta) can minimize the damage caused by stroke and improve patient outcome in patients up to ten hours after the onset of their stroke.
The study is a prospective, controlled, randomized, multi-center study of NeuroFlo treatment plus standard medical management versus standard medical management alone. Randomization will be 1:1 and stratified to ensure equivalent patient distribution for stroke severity and duration. The primary efficacy endpoint is 90 day neurological and functional status. Additional endpoints include safety, perfusion enhancement, 24 hour neurological status and quality of life.
Eligible subjects are men and women aged 18-85 with symptoms of an ischemic stroke. NIHSS neurological status score must be between 5-18 and time from symptom onset less than ten hours. A minimum of 100 and a maximum of 244 patients may be enrolled in each study arm based on statistical significance of the results. Patient enrollment began in late 2005 and will continue into 2008. To date, nearly 40 North American sites have committed to participate in the trial.
Dr Harish Shownkeen, Director of Endovascular Surgical Neuroradiology at Central DuPage Hospital treated the first patient in the SENTIS trial. Shownkeen commented, “This patient had no proven acute treatment options, due to the relatively long time from the onset of symptoms to treatment. The NeuroFlo catheter was deployed easily and treatment occurred with no issues. We are pleased to have enrolled the first patient in this unique and important trial.”
10-24 hour strokes
CoAxia, in conjunction with several leading stroke centers, has co-authored an additional protocol to test the feasibility of treating patients with the NeuroFlo catheter out to 24 hours after the onset of a stroke, potentially making this an option for victims who suffer their stroke while sleeping or otherwise do not seek treatment for several hours. This study, called Flo24, is designed to be a safety/feasibility study to assess the safety of treating late presenting stroke patients who demonstrate an ischemic penumbra in an MRI perfusion scan.
Cerebral vasospasm
In 2005, CoAxia received FDA approval for the NeuroFlo Catheter to treat patients with cerebral vasospasm under a Humanitarian Device Exemption. The Model 1017 NeuroFlo catheter is approved for the treatment of cerebral ischemia resulting from symptomatic vasospasm following aneurismal subarachnoid hemorrhage (SAH), secured by either surgical or endovascular intervention for patients who have failed maximal medical management.
Data on vasospasm patients treated with the NeuroFlo catheter demonstrated a complication rate consistent with this severely ill population as well as indications of potential benefit via 50% of patients showing an acute neurological improvement of four points or greater in the NIHSS scale.
Along with this recent US release of the HDE-approved catheter, CoAxia is making available a patient data and outcomes registry. The objectives of the registry are to gather data demonstrating perfusion augmentation in symptomatic vasospasm patients treated with NeuroFlo, and to gather data regarding clinical outcome.
In addition to stroke, planning is ongoing for clinical feasibility studies to evaluate the potential of CoAxia’s perfusion augmentation technology for other cerebral, cardiac and renal applications.
Andrew M Weiss, president and CEO of CoAxia commented: “We are pleased that we now have three stroke studies underway at several of the top stroke institutions in North America evaluating our NeuroFlo technology in patients from 0-24 hours post stroke. CoAxia is committed to evaluating and bringing its perfusion augmentation therapy to the large and significantly undertreated population of stroke victims.”