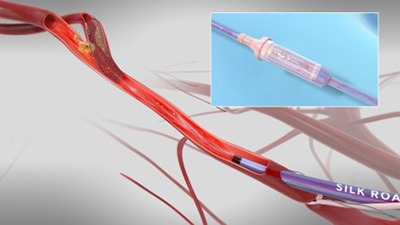
Six presentations on Silk Road Medical’s Enroute transcarotid neuroprotection and stent system were given at the Society for Vascular Surgery annual meeting (8–11 June, National Harbor, USA).
Christopher Kwolek, director of the vascular and endovascular training programme at Massachusetts General Hospital, chief of Vascular Surgery at Newton Wellesley Hospital, Newton, USA, and national co-principal investigator for the ROADSTER trial, presented “TransCarotid artery revascularisation with high-rate flow reversal embolic protection demonstrates improved stroke and death rate following FDA premarket clearance.” Kwolek presented a 30-day all stroke rate of 1.3% from the continued access cohort of patients from the ROADSTER trial, which consisted of an additional 78 high surgical risk patients enrolled beyond the pivotal cohort of 141 patients while the premarket clearance application was under review by the US Food and Drug Administration (FDA). This compares to a 30-day all stroke rate of 1.4% in the pivotal cohort, for a combined rate of 1.4% in 219 patients. The 30-day stroke and death rates were 2.8%, 1.3% and 2.3% in the pivotal, continued access, and combined cohorts, respectively. Kwolek commented that “the combined outcomes in high surgical risk patients are remarkably better than high surgical risk patients treated with conventional carotid endarterectomy (CEA).”
Ignacio Leal, Complejo Hospitalario de Toledo, Spain, whose site was the leading enroller in the ROADSTER study, presented “One-year follow-up after transcarotid artery revascularisation (TCAR) with Enroute transcarotid neuroprotection system.” Leal presented a cohort of 50 consecutive patients, including patients enrolled before and within the ROADSTER trial, and reported no strokes or deaths at 30 days with a 12-month stent patency and stroke-free survival rate of 100%. Leal concluded that “TCAR can be done with a high rate of technical success, an extremely low rate of major adverse events, and excellent one-year stroke-free survival and stent patency.”
Ann Kim, University Hospitals Case Medical Center, Cleveland, USA, presented a poster titled “Temporary reversal of blood flow during transcarotid revascularisation (TCAR) does not change brain electrical activity” on behalf of her colleagues at Case Medical Center, University of California Los Angeles School of Medicine, Los Angeles, USA, and State University of New York, Buffalo, USA. Kim reported that 28 patients enrolled in the ROADSTER trial underwent electroencephalogram (EEG) monitoring during TCAR with nine patients having bilateral carotid artery disease including four of nine with contralateral occlusion. No EEG or somatosensory evoked potentials (SSEP) changes or adverse events occurred during the implementation of the Enroute device in all patients. Furthermore, none of the patients exhibited changes in their pre- and post-intervention neurologic physical exam or their NIH stroke scale (NIHSS). Kim concluded, “Reversal of flow did not elicit any change in brain electrical activity, even in patients with bilateral carotid disease. This finding, coupled with the unchanged post-operative neurologic exam, suggests that temporary reversal of flow is safe. Carotid stenting performed with carotid artery reversal of blood flow can mitigate carotid embolisation without causing brain ischaemia.”
Vikram Kashyap, professor and chief, Division of Vascular Surgery, University Hospitals Case Medical Center, and co-principal national investigator for the ongoing ROADSTER 2 study, led an SVS/ESVS (European Society of Vascular Surgery) joint debate session titled “During carotid artery stenting, retrograde flow is better than filter-based embolic protection devices for the prevention of embolic stroke.” In his presentation, Kashyap commented that “the very nature of TCAR and its direct carotid approach significantly reduces the risk of stroke, since it does not require embolegenic steps like traversing the aortic arch and the carotid lesion with wires and catheters before implementing neuroprotection. It is simply a more logical approach.”
TCAR with the Enroute system was also featured in a “Vascular Live” presentation titled “TransCarotid artery revascularisation (TCAR): The way forward in treating carotid artery disease and stroke prevention,” featuring Kashyap, Raghu Motaganahalli, associate professor, Indiana University, Indianapolis, USA, and Peter Schneider, chief, Division of Vascular Therapy at Kaiser Foundation Hospital in Honolulu, USA, and co-principal national investigator of the ongoing ROADSTER 2 post-approval study. During the session Schneider commented that “ROADSTER 2 is enrolling faster than we anticipated in a broad group of centres including many sites where TCAR has just recently been adopted. There is a high level of enthusiasm for the procedure and this experience will build upon the compelling evidence base from ROADSTER 1.” Schneider and Kashyap also led a pre-course education session titled that featured TCAR and the Enroute system.
Silk Road Medical’s chief medical officer Sumaira Macdonald, commented that “the robust evidence base continues to build for TCAR as a compelling alternative to both carotid endarterectomy and transfemoral carotid artery stenting. With such low peri-procedural stroke rates and the benefit of a less invasive approach, TCAR has the clear potential to be standard of care in the treatment of carotid artery disease.”













