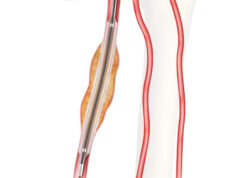
Interim twelve-month data from the Lutonix AV Clinical Trial indicate that treatment of dysfunctional arteriovenous (AV) fistulae with Bard’s Lutonix drug-coated balloon (DCB) produces non-inferior safety outcomes and a 37% improvement in primary patency when compared with plain percutaneous transluminal angioplasty. Scott Trerotola (Philadelphia, USA) also told delegates at the 2017 Charing Cross Symposium (CX; 25–28 April, London, UK) that the data suggest a sustained efficacy benefit, which will be further explored as the trial continues out to 24 months.

Last year marked the 50th anniversary of the AV fistula, Trerotola said. “It is interesting to note that in the half century since, while there have been a large number of multicentre, randomised trials comparing devices with angioplasty in grafts, to date there has not been a large, multicentre, randomised trial looking at an intervention to prevent restenosis in fistulae until now.”
The prospective, global, multicentre, randomised Lutonix AV Clinical Trial was designed to assess the safety and effectiveness of the Lutonix 035 paclitaxel-coated balloon catheter in the treatment of dysfunctional AV fistulae. Enrolling 285 randomised subjects at 23 clinical sites, the primary effectiveness endpoint is target lesion primary patency at six months, while the primary safety endpoint is freedom from any serious adverse events involving the AV access circuit out to 30 days.
The patient cohort was a “real-world” group. Patients had to be ≥21 years old with upper extremity AV fistulae exhibiting clinical, physiological or haemodynamic abnormality. The fistulae had to be at least one month old and have undergone at least one haemodialysis session. The fistulae had ≥50% stenosis, were ≤10cm long, had successful pre-dilation, and were of diameter 4–12mm. Exclusion criteria included lower extremity access, thrombosed access and symptomatic central venous stenosis, as well as symptomatic restenosis in stents or stent grafts in the circuit. Patients were excluded if they had more than two lesions in the circuit, a secondary non-target lesion that could not be successfully treated, or central veins as a secondary lesion.
Explaining the treatment process, Trerotola noted, “We believe we have to get a good angioplasty before we apply the drug. We used ultra-high-pressure angioplasty to get the good result initially and to get the acute gain needed.” Following this, patients were randomised 1:1 to either Lutonix DCB catheter treatment or standard balloon angioplasty.
Demographics were similar between groups, with hypertension, diabetes and coronary artery disease relatively common in both groups. Trerotola noted that there were a low number of smokers. Fistulae location “reflects a US population, with two thirds in the upper arm and one third in the lower arm, which is the opposite of what you would see in Europe,” he continued. There was no difference in treatment benefit between groups for fistula location.
There was “a good distribution” of various types of lesions, Trerotola said. Most lesions were at inflow (33.8% DCB and 29.6% PTA), outflow (24.5% DCB and 22.5% PTA), or cephalic arch (18.7% DCB and 22.5% PTA).
Approximately a third of lesions in both groups were de novo (30.5% DCB vs. 27.1% PTA) and mean target lesion length was 28.4±15.09mm in the DCB group and 29.5±18.69mm in the plain angioplasty group. Tandem lesion rate was 2.8% in the DCB group and 7% in the plain balloon group.
“The primary safety outcome measure was met at 30 days, and since then we have seen that the two groups are essentially exactly matched,” Trerotola reported. Target lesion primary patency, on the other hand, was shown to be 37% better in the DCB group at 12 months, with the divergence beginning at approximately 60 days. At the primary patency endpoint of exactly six months, the difference was not statistically significant, although Trerotola described that as “a statistical blip” given that it was significant at later time points. “It is plain to see that there is a sustained and significant benefit of the drug over plain balloon angioplasty,” Trerotola concluded.
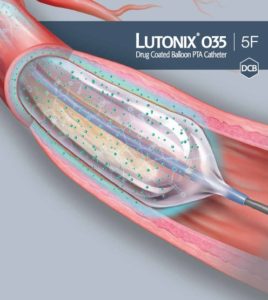 Lutonix DCB Global Real World BTK Registry
Lutonix DCB Global Real World BTK Registry
In another session at CX 2017, Andrej Schmidt (Leipzig, Germany) presented the most current interim six-month results of the Lutonix DCB Global Real World BTK Registry, reporting the 30 day safety and six-month target lesion revascularisation rate.
The prospective, multicentre, single-arm Registry was designed to assess the clinical use, outcomes and safety of Lutonix when used to treat native below-the-knee arterial lesions in a heterogeneous patient population. The trial will enrol up to 500 patients in 35 international sites and follow them out to 24 months. All patients will have Rutherford classification 3–5, ≥70% lesion stenosis and target vessel(s) reconstituting at or above the ankle with inline flow to at least one patent vessel.
At 30 days, the primary composite safety endpoint was met in 98.2% of cases, and in 95.1% at six months. Freedom from all-cause death was 89.8%, freedom from major amputation was 95.6%, freedom from re-intervention for thrombosis/thrombolysis was 95%, freedom from reintervention for distal embolisation was 99.2%, freedom from target vessel revascularisation was 85.8%, and freedom from unexpected device or drug-related event was 100%.
The other endpoint—freedom from target lesion revascularisation—was 98.7% at 30 days and 86.2% at six months.
“These interim results really look quite promising with the high rate of freedom from target lesion revascularisation and the low amputation and distal embolisation reintervention rates,” Schmidt said.
Schmidt told the audience that the Lutonix below-the-knee investigational device exemption (IDE) trial is also currently in progress, and will compare the DCB to plain balloon treatment. It will enrol up to 840 randomised subjects at 75 global sites. So far, 382 subjects have been randomised and the current major amputation rate is 3.2%.