Atul Gupta, MD, Interventional Radiologist and Chief Medical Officer, Philips Image Guided Therapy

Our roles as interventionalists have been transformed over the past 20 years. With the growing and aging population and rise in chronic, lifestyle-related diseases the number and complexity of image guided procedures carried out in interventional labs has changed enormously – drastically influencing the day-to-day clinical experiences of interventionalists across a range of specialities.
Driving the change
Our aging population means people aged 60 and over comprise the fastest growing age group worldwide. By 2030 over a billion more lives will have been added to our planet.1 Behavioral risk factors such as tobacco use, unhealthy diet, insufficient physical activity and alcohol use, have and will continue to lead to an increase in chronic diseases, such as cardiovascular and respiratory disease, cancer and diabetes.
As a result of these population changes and the rise in chronic diseases, there has been an increase in the number, range and complexity of interventional procedures we carry out each day.
Achieving more with less
At the same time, nearly all of us are acutely aware, often first hand, of the co-existent healthcare resource constraints that exist. All interventionalists are now expected to do more with less. A frequent refrain I hear from my fellow physicians is how can we deliver improved outcomes to more patients, with increasingly complex patient cases, all while reducing procedure time and hospital stay?
Fortunately, improvements in technology, including the development of intuitive systems and suites, standardization of procedural workflow and seamless integration of smarter devices, will support the next generation of interventions, allowing us quite simply, to do more, do it better, and do it faster. Improvements in image guided therapy technology will result in even less invasive procedures, fewer repeat procedures and improved workflow.
We are already seeing an evolution in procedures that once required lengthy hospitalization, which can now be conducted in an out-patient setting or even an office-based lab. Reducing the length of hospital stay frees up valuable hospital resources, saves cost, and allows us to treat more patients – bringing significant financial efficiencies.
 A look to the future
A look to the future
It’s no surprise that advances in image guided therapy have already increased the number and range of procedures each interventionalist can carry out. My typical case mix and load has changed dramatically over the past two decades. But I have also seen technology follow suit, giving me new image guided navigation tools, at low radiation doses with improved image quality and reduced contrast requirements.
Compare the interventional lab of 20 years ago, equipped with basic X-ray and fluoroscopy tools, with the full hybrid suites of today. I am very excited to see how the newest systems are providing comprehensive procedural solutions such as imaging and navigation optimized, for instance, for interventional oncology applications or Transcatheter Aortic Valve Replacement (TAVR) procedures.
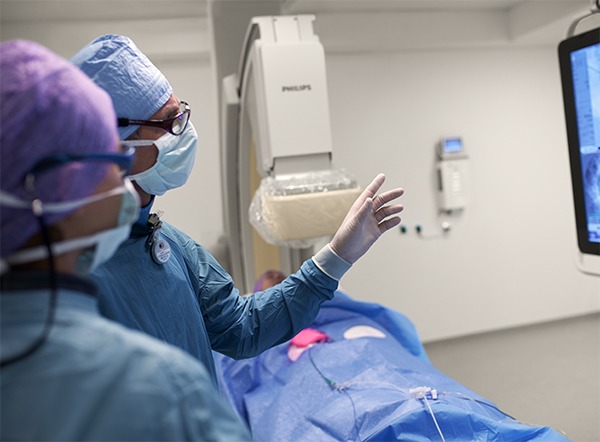 Developing more intuitive systems is crucial, as complexity can be a significant barrier preventing physicians from using new technology; if technology and interface are not elegant, user-friendly and fast they will not be used. The system should feel like an extension of the physician’s hand and mind, and little thought should need to go into figuring out how to operate it; we prefer to concentrate on our patient. Easy-to-use systems have the potential to make image guided therapy simpler and faster, and improve both the patient and physician experience.
Developing more intuitive systems is crucial, as complexity can be a significant barrier preventing physicians from using new technology; if technology and interface are not elegant, user-friendly and fast they will not be used. The system should feel like an extension of the physician’s hand and mind, and little thought should need to go into figuring out how to operate it; we prefer to concentrate on our patient. Easy-to-use systems have the potential to make image guided therapy simpler and faster, and improve both the patient and physician experience.
Standardization of workflow will have the potential to also improve not only the time it takes to complete each case but also patient outcomes. While no two patients and no two interventions are exactly the same, there is still room for some procedural standardization to improve workflow and consistency of care, and ensure the best patient outcomes are delivered as often as possible.
Improvements in workflow will also come from the integration of the equipment contained within the interventional lab. It is not uncommon, and often typical during an intervention for physicians to consider and analyse data from numerous sources, such as hemodynamic data, electronic health records, historic imaging such as from computerized tomography (CT) scans, live 2D fluoroscopy, 3D navigation imagery, intravascular ultrasound (IVUS) and device information such as iFR or ablation catheter data. Each is shown on an individual screen. Obviously a seamlessly integrated system showing all of the relevant data together in a contextual relevant manner, would improve lab performance, and allow for more efficiency.
In the face of global healthcare challenges and resource constraints it is crucial that the technology in interventional labs is flexible and efficient, standardized, intuitive and easy-to-use, to help us interventionalists meet the unprecedented demands we face now, and in the future.
References
1. United Nations, World Population Prospects, Key Findings and Advance Tables, 2015. Accessed November 2016. Available https://esa.un.org/unpd/wpp/publications/files/key_findings_wpp_2015.pdf
This advertorial was first published in Vascular News Issue 73, January 2017.













