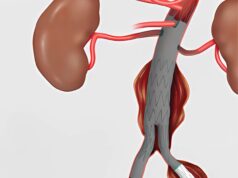
At the 2005 Multidisciplinary European Endovascular Therapy (MEET) meeting, Patrice Bergeron of Saint Joseph Hospital, Marseille, France discussed the role of hybrid procedures for acute type A dissection.
He started by claiming that an acute type A dissection is an emergency for all patients and has a high morbidity and mortality for associated arch dissection. However, a stentgraft is a recognised action for high-risk patients with complicated acute or chronic type B aortic dissection. In addition, Bergeron noted that chronic dissections extending to the aortic arch may benefit from the hybrid treatment.
Although surgical treatment remains the current gold standard, Begeron said the current mortality rate is between 8-17% (Svenson-Fattori) with a 10-year survival rate of 42%. Moreover, there is a re-operation rate of 27% where the diameter has increased. The factors attributing to a poor survival rate include those patients aged 70 or more, with a laceration of the aortic arch and those with renal ischaemia. In addition, those patients who receive medical therapy are limited to a poor survival rate. Although surgical repair with hypothermic cardiac arrest cerebral perfusion is the gold standard for young patients, it is not benign for high-risk patients. Finally, the emergence of branched stent grafts are experimental for thoracic aortic aneurysms and not applicable to acute type A dissection.
As a result of these shortcomings, Bergeron highlighted the emergence of a hybrid procedure. The current management of acute arch dissection depends on the mechanism for dissection; a retrograde dissection from Type B dissection can be treated with surgery or stentgraft in the descending aorta. However, an antegrade type A dissection can be treated with surgery (depending on the location of the intimal tear and extension of disease), repair of the ascending aorta alone, combined aortic valve replacement + Coronary Artery Bypass Grafting +/- Bentall, arch replacement with elephant trunk or a combined treatment for high-risk patients.
However, type A dissection can be unfit for arch replacement, either due to the absence of the proximal tear of an unknown origin or as the tear extension to the arch in high-risk patients is unfit for arch surgery. Therefore, Bergeron recommended ascending aorta replacement and a combined bypass to IA (right hemi-arch transposition), followed by staged arch stentgrafting with/or carotido-carotid bypass.
This staged hybrid treatment for acute type A dissection is safe and feasible for high-risk patients and respects life salvage by ascending aorta replacement. Moreover, Bergeron claims this treatment avoids complex arch repair, reduces the morbidity and mortality of arch extended dissection and allows centres not used to arch surgery to perform a simple procedure.
Also at MEET, Dr Dierk Scheinert, director of the Department of Angiology, Heart Center Leipzig, Germany, presented on the Cypher-BTK-Pilot Study. The prospective, non-randomised, monocentric study looked at sirolimus-eluting versus bare-metal balloon-expandable stents for symptomatic infrapopliteal obstructions.
Inclusion criteria for the study, which had a sample size of 60 patients, was Symptomatic Peripheral Arterial Occlusive Disease, single infrapopliteal lesions, lesion length up to 30mm and reference vessel diameter 3-3.5mm. Inflow lesions (iliac of femoropopliteal) need to be treated prior to index procedure.
Thirty patients were treated with the sirolimus-eluting Cypher select stent and 30 – in the control group – with the Sonic bare-metal stent. Antiplatelet therapy was carried out for six months with ASA 100mg/d and Clopidogrel 75 mg/d.
Of the patients in the Cypher group the mean age was 71.4 and 56.7% were male. Eighty-three point three per cent had Diabetes Mellitus, 96.9% had material hypertension and 30% were smokers. Of the control group, 63.3% were male and the mean age was 73. Seventy-six point six had Diabetes Mellitus, 100% had material hypertension and 36.6% were smokers.
Scheinert said according to the study’s angiographic follow-up the use of sirolimus-eluting stents was associated with a significantly reduced in-stent-reobstruction rate (0% vs 56%). Adverse clinical events (amputation and TLR) could also be significantly reduced using sirolimus-eluting stents.
In conclusion he said both concepts – Bio-absorbable Mcalloy-stents and Sirolimus-eluting stents – were safe and effective for treatment of focal infrapopliteal obstructions. However, he added that these results need to be validated in randomised, multicentric trials.
As part of the lower limb arteries session at MEET, Dr Thomas Sos, New York Presbyterian Hospital institution, made a presentation titled, ‘The indications for techniques and results of renal angioplasty and stenting in patients with ischaemic nephropathy’.
In this study, 94 Palmaz stents were placed in 84 patients between May 1992 and September 1997 at the New York Presbyterian Hospital Weill Cornell Center. A total of 88 stents were placed for ostial lesions, 77% primarily in ostial lesions or total occlusions and 28% after previously failed angioplasties. The indications for intervention were: hypertension (96%), renal failure (60%) and recurrent flash pulmonary oedema in 30% of patients (many patients had multiple indications). A total of 98% of procedures were successful.
Sos reported that angiographic follow-up has been performed in 36% of implanted stents and demonstrated that 78% of the stents were widely patent, 22% of stents showed 60% restenosis, with one patient dying prior to follow-up from an unrelated cause. Clinical follow-up was available in all patients at a mean of 19 months and in 40 at more than 15 months.
The mean blood pressure prior to stenting was 183/91mm Hg and at the latest follow-up was 149/78mm Hg, whilst the number of antihypertensive medications was reduced from a mean of 2.93 +1.4 to 2.63 +1.3. In addition, Sos reported that 11 of 13 patients with recurrent flash pulmonary oedema and bilateral renal artery stenosis were cured following stenting of one of both renal arteries.
Sos concluded that for patients with physiologically significant renal artery stenosis, renal artery stenting is the treatment of choice for renal dysfunction, poorly controlled hypertension or recurrent pulmonary oedema with immediate mid-term results similar to open surgical repair.
However, Sos concluded that there is no evidence that prophylatic stenting of mild to moderate, physiologically non significant and clinically asymptomatic stenosis (especially if not fully evaluated) renal artery stenosis has any benefit compared to aggressive medical therapy and life style changes to prevent progression and clinical squeal of renal failure, hypertension and decreased longevity.