In the last 20 years, there have been major developments in the use of endovascular and hybrid haemorrhage control tools, especially in the treatment of ruptured abdominal aortic aneurysm (rAAA).
It has been shown that total endovascular aortic repair (EVAR) for rAAA is feasible, with good results from the use of endovascular and hybrid methods and tools (Mayer et al. Annals of Surgery 2012). Use of embolisation, endografts, balloons and other tools for bleeding control has grown rapidly as well, and these methods are now also being used for gastrointestinal, tumour, iatrogenic and medical bleeders and post-partum bleedings. Endovascular methods developments have not been limited to bleeding patients, but also expanded to other fields, with the use of extracorporeal membrane oxygenation (ECMO) and the evolving eCPR concept for cardiac arrest.
The collection of tools described here can be subsumed under the recently established concept of endovascular resuscitation and trauma management (EVTM). It requires a multidisciplinary platform on which surgeons, vascular surgeons, interventionists and ICU and trauma surgeons work together on the unstable patient from arrival to the achievement of effective haemorrhage control and resuscitation. Indeed, the use of endografts for traumatic thoracic aorta bleeding, and bleedings in subclavian and other major vessels, is in use today in trauma, as it is in embolisation for visceral bleedings and pelvic bleeding in trauma patients resuscitative endovascular balloon occlusion of the aorta (REBOA), or aortic balloon occlusion (known as ABO, or I-ABO), has been used for many years in vascular surgery, and is a part of the endovascular arsenal, with a crucial role in unstable patients with rAAA. In the last eight to 10 years, endovascular techniques including REBOA have expanded into trauma surgery, with major application to patients with non-compressible torso haemorrhage (NCTH) in both the hospital and an austere or military environment. NCTH is a major cause of death, both in civilians and from military injuries, and an open-surgery approach and damage control have for many years been the gold standard. Lately, with increasing use and limited reports and studies, REBOA has gained popularity (and also given rise to substantial controversy) in the trauma world.
REBOA has now been adopted in some practical trauma guidelines; and, for example, pelvic traumatic bleeding has, to some extent, replaced thoracotomy or laparotomy and open aortic clamping (Figures 1 and 2).
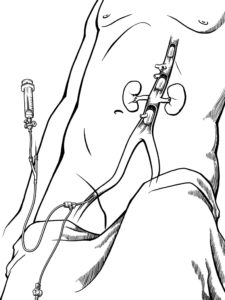

While endovascular technology evolved in the last 10 years, imaging has also undergone tremendous developments. Computed tomography (CT), ultrasound, hybrid suites and other imaging modalities have become faster and more accurate, specific and accessible in many centres. Historically, just several years back, CT may have been regarded in the trauma world as “the tunnel of death” due to long scanning time and availability as well as its location. It is still a common belief and praxis that embolisation necessitates transfer of the patient and long procedure times. The introduction of EVTM multidisciplinary collaboration, as well as modern endo tools and imaging, hybrid suites and the emerging CT-on-rails and hybrid ER, now allows the fast use of minimally invasive methods, immediately on patient arrival, in one place with minimal delay.
The EVTM concept is still developing, and hard data supporting its benefits have not yet been presented. In some areas in trauma, however, the use of minimally invasive tools is clearly supported by data, as in the cases of treatment for thoracic aortic injuries and embolisation for pelvic bleeding (as mentioned above). REBOA for NCTH is not yet established, and, so far, there are no prospective randomised data to support its widespread use. As EVTM develops to include also no-bleeders and resuscitation, there is a great need for the multidisciplinary evaluation and implementation of methods such as REBOA and ECMO, as other endo or hybrid techniques. There are some ongoing studies that we hope will supply firmer data in the coming two years. There is also massive work on the development of the EVTM concept and its recognition. This has been achieved partially by the EVTM symposiums (four meetings done by Dec 2018, with two more planned for 2019), workshops, seminars, registry studies, animal studies, multicentre studies and the Journal of Endovascular Resuscitation and Trauma Management (JEVTM), as well as by the expanding EVTM community. All the activities have aimed at sharing and gathering data to support medical practice and science.
The motto of the EVTM movement is simple: “no ego, just good science and cooperation”. Vascular surgeons and interventional radiologists should play the leading role in using these methods clinically as needed, and in the gathering and sharing of data to support or reject their application to our patients.
Tal Hörer is a Vascular and General surgeon at the Örebro University hospital in Örebro, Sweden, founder of the European EVTM Symposium, and editor-in-chief of JVETM.













