 A new Expert Panel Report, published in The Diabetic Foot Journal, recommends a new treatment algorithm for topical oxygen therapy in patients with diabetic foot ulcers (DFU). The new treatment algorithm recommends that topical oxygen therapy is considered as an adjunct to standard of care after four weeks if the wound area has not reduced by 40%. In addition, it recommends that early initiation (<4 weeks) of topical oxygen therapy could be beneficial for patients where peripheral arterial disease (PAD) is present, where there is ulcer pain, non-healing after amputation, or sloughy wounds.
A new Expert Panel Report, published in The Diabetic Foot Journal, recommends a new treatment algorithm for topical oxygen therapy in patients with diabetic foot ulcers (DFU). The new treatment algorithm recommends that topical oxygen therapy is considered as an adjunct to standard of care after four weeks if the wound area has not reduced by 40%. In addition, it recommends that early initiation (<4 weeks) of topical oxygen therapy could be beneficial for patients where peripheral arterial disease (PAD) is present, where there is ulcer pain, non-healing after amputation, or sloughy wounds.
There are approximately 169,000 people with a DFU in the UK, with nearly 65% complicated by PAD, presenting a treatment challenge. The Expert Panel Report states that advanced treatment options are needed as healing rates under standard-of-care are often poor. Oxygen is known to be essential for wound healing. Sustained delivery of oxygen, either from the blood supply or applied from an external source such as topical oxygen, is vital to heal non-healing wounds, especially for DFUs, often complicated by PAD.
Paul Chadwick, Visiting Professor at Birmingham City University and chair of the Expert Panel Report, commented: “The evidence for topical oxygen therapy is growing and is shown to be beneficial and improve outcomes in suitable patients. This new consensus document and simple treatment pathway provides clarity on the role of topical oxygen therapy and when it should be introduced to help manage and heal these difficult to heal wounds. The patients of biggest concern for me are those with severe ulcers as they are four times more likely to need a major amputation and almost twice as likely to die within one year.”
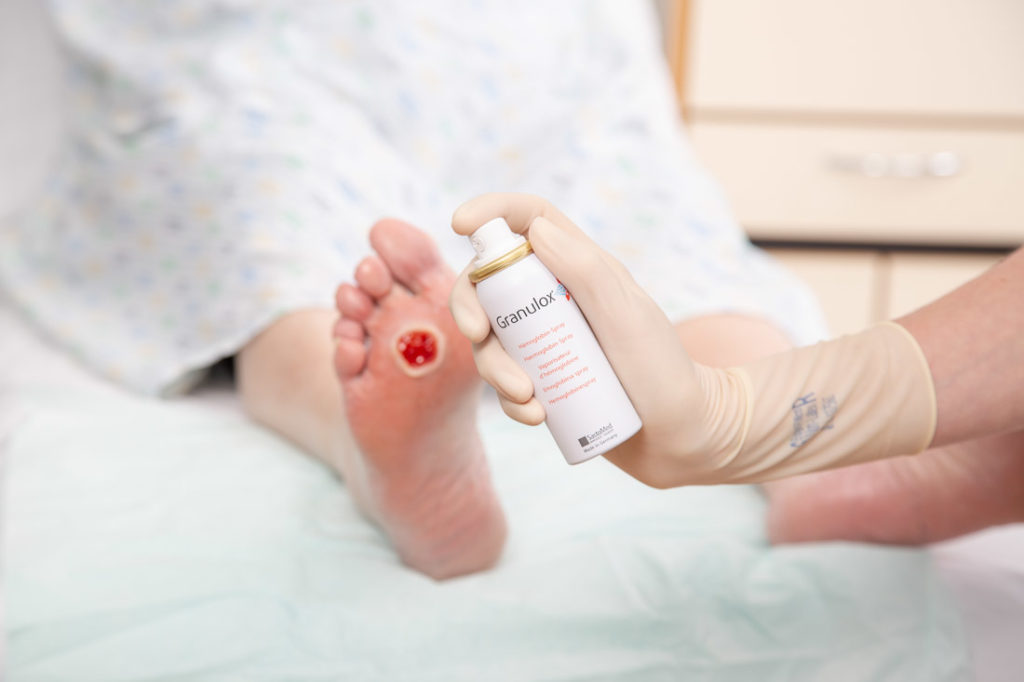
One product showing promising results in topical oxygen therapy is Granulox (Mölnlycke), a haemoglobin spray that binds oxygen from the atmosphere and transports it to the wound bed, where it is released.
A European Wound Management Association (EWMA) evaluation of the currently available oxygen therapies in wound care awarded the haemoglobin spray a treatment recommendation of Grade 1B, indicating a positive benefit–risk value with moderate quality of evidence and very strong observational studies.
In a single-blinded randomised controlled trial on 72 patients with venous leg ulcers, the average wound size reduction was 53% at 13 weeks (p<0.01) in the group treated with the haemoglobin spray. No statistically significant reduction in wound size was seen in the control group. Several studies have shown a reduction in DFU size when haemoglobin spray is used as an adjunct to standard care.
Studies have also shown that twice as many chronic wounds healed at 8–16 weeks with the haemoglobin spray compared to standard of care, with shorter time (50%) to heal. More than 70% of patients have reported lower average pain scores at four weeks with the haemoglobin spray than with standard of care in chronic wounds, and 99% have shown less slough in chronic wounds after four weeks compared to 33% with standard of care.
The Expert Panel report advises that initiation of topical oxygen therapy for the treatment of DFUs should be undertaken by the multidisciplinary foot care service or a clinician experienced in diabetic foot care; it can then be continued in the community.
Diabetic foot disease is the largest single reason for hospital admissions among people with diabetes. DFUs cost the NHS an estimated £1 billion per year, while the additional social costs to the patient, such as reduced mobility and sickness absence, are estimated at £13.9 billion per year. The indirect, intangible costs people with diabetic foot disease are also high, with many experiencing a poorer quality of life than those without foot disease. In total, 85% of amputations are preceded by a DFU, people who develop a DFU are also at greater risk of premature death, myocardial infarction and fatal stroke than those without a history of DFUs.
DFUs have a significant impact on patients, and the expert panel concluded that topical oxygen therapy should be considered as an adjunct to best practice for DFUs due to its ability to improve outcomes in patients.













