An important session on day three of CX Aortic Vienna (24–26 October, Digital) reframed the focus from intervention to conservative treatment in highly defined aortic arch patients. Roger Greenhalgh (London, United Kingdom) noted that it was “mighty difficult to find a circumstance in the aorta where you can sit tight, with certainty, that the patient will be safe”. Michel Makaroun (Pittsburgh, United States) remarked, “[this session] really reminds clinicians that the answer is not always an intervention in 100% of patients.”
Makaroun submitted that a treatment strategy should never be “a knee-jerk reaction”. “You always have to evaluate what you have to offer and whether it is going to be for the benefit of the patient. There are many instances where you can wait. You may still have to intervene later, probably electively, when the situation is more appropriate, or occasionally you might not have to intervene at all. So, I think this is a reminder to all of us that the answer is not always to take the patient quickly to the operating room,” he said.
Greenhalgh then pointed to the “uphill battle” of trying to define circumstances and situations in which an immediate operation is not required. A trio of presentations then attempted to do just that. Makaroun kickstarted the series of presentations that argued that non-operative management can best serve selected patients with arch injury.
In 2007, the American association for the Surgery of Trauma (AAST) reported a “major shift” in treatment strategy for blunt thoracic aortic injuries away from open surgery towards thoracic endovascular aortic repair (TEVAR). And that swing was based on decreased mortality and paraplegia rates, he said.
“Although TEVAR was becoming the standard of intervention, a review of national trends revealed that non-operative management was still being used to treat 54% of patient in 2011. This proportion decreased to around 28% in the period between 2016 and 2019,” he clarified.
The only published guidelines (Society for Vascular Surgery, 2011) recommend non-operative management for grade I injuries and TEVAR for grades II, III and IV, but more recent data suggests that grade II injuries are also relatively benign, clarified Makaroun. “Heterogeneous injury characterisation and variable follow-up remain major limitations to the use of non-operative management across all grades of blunt trauma injury,” Makaroun said.
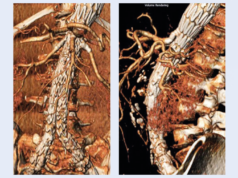
A review published this year of 192 patients in whom non-operative management was compared with TEVAR showed at three-year follow up that none of the 64 patients treated with non-operative management developed a progression of the lesion and that immediate outcomes were comparable. In the study there were 14 patients with grade III injuries treated conservatively due to location or associated trauma and interestingly these did not progress at the three-year mark, either, noted Makaroun.
“Traumatic aortic transection can be managed conservatively in many patients,” he said, commenting that while TEVAR is an excellent treatment for significant blunt thoracic aortic injury, non-operative management is a safe and best treatment for minimal aortic injury grades I and II. It can safely be used for select grade III injuries when TEVAR is not easily applicable or is not an immediately available option,” concluded Makaroun.
Then, Maani Hakimi, Lucerne, Switzerland, turned tack to describe therapeutic strategies for mycotic penetrating aortic ulcerations. “The recommendations for penetrating aortic ulcerations with signs of acute complications are clear and management according to acute aortic dissection is recommended,” he said, sharply contrasting this approach with asymptomatic and uncomplicated penetrating ulcers that see variable treatment. Current publications show a trend towards conservative treatment in this latter group, said Hakimi, because in this group low growth and low rupture rates have been observed. Rapid expansion and secondary complications such as infection, symptom development or rupture necessitate interventional treatment, he cautioned. The ensuing discussion centred on the critical importance and difficulty in correctly diagnosing mycotic penetrating aortic ulcerations.
Ottavia Borghese (London, United Kingdom) then dwelt on the early and long-term outcomes in the treatment of type non-A non-B aortic dissection in a single centre. In such patients, Borghese emphasised, the benefits of best medical therapy or surgical treatment depends critically on selection criteria based on clinical and radiological findings. After calling for larger datasets to provide definitive conclusions, Borghese said: “[…] We see a trend towards an enlarged initial diameter of descending aorta seems to be related to both an early and late intervention. Frozen elephant trunk provides immediately satisfactory results and false lumen thrombosis in most patients.”