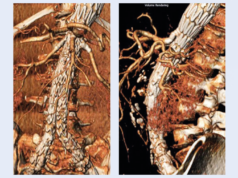
While the long-term durability of fenestrated endovascular repair (FEVAR) has been established, the need for accurate procedural planning may act as a barrier to widespread adoption. At the 2016 VEITHsymposium (15-19 November, New York, USA), Benjamin Starnes, University of Washington, Seattle, USA, suggested that this barrier may be overcome thanks to AortaFit automated planning software.
“FEVAR is an established and durable endovascular option for short neck/juxtarenal abdominal aortic aneurysms,” Starnes told delegates, and has shown “low rates of long-term aneurysm-related morality, sac expansion and rupture, branch vessel occlusion, type Ia endoleak and open conversion.” Despite these advantages, the time, expense and complexity of case planning present a significant challenge, especially in angulated anatomy. Moreover, even when FEVAR is available and a centre is able to complete the required planning, it is still subject to human error.
Aortica’s three-platform technology may offer a solution to these issues, Starnes said. The first stage uses AortaFit software, in which a patient’s computed tomography (CT) scan is analysed to determine fenestration coordinates. In the second stage, the endograft is manufactured via a “precise fenestration alignment” process with patient-specific reinforced and circumferentially radiopaque fenestrations placed on the graft. Third comes the expansion of a unique, purpose-built branch stent (Boulevard stent) that is designed to engage with the fenestration. This can be achieved in one step with fewer catheter and wire exchanges than other fenestrated procedures, Starnes explained. There is no secondary flaring of the proximal end of the branch stent, minimal stent is left in the flow channel, and no secondary bridging stents would be required. “Simplified fenestrated endograft deployment” is thus achieved.
AortaFit software is currently being evaluated in an ongoing US Food and Drug Administration physician-sponsored IDE study at the University of Washington. Starnes presented results from an ongoing trial of the AortaFit in patients with juxtarenal aortic aneurysms deemed unsuitable for open repair. For the first 10 patients treated, technical success was achieved in nine (90%). Graft modification time was “very respectable” at 54.4±5.7 minutes and mean fluoroscopy time was 37±18 minutes.
At thirty days, there had been major adverse events in two patients (one non-ST-elevation myocardial infarction and one minor ischaemic stroke). Mortality was 0%, mean length of intensive care unit stay was 1.5±0.9 days and mean total hospital stay length was 2.3±1.4 days. There was no type I or type III endoleak, and branch artery patency was 100%. There were no major adverse device events. A total of 20 patients have been treated to date.
“In the [Pacific Northwest Vascular Study Group], we perform more than 80% of complex EVAR, and we have the best results in the nation, according to VQI,” Starnes said. “We have the best procedure time, the best levels of estimated blood loss, some of the best postoperative complication rates and the lowest rates of complex major cardiac events. Importantly, we are the best at returning our patients to the pre-surgical care setting.”
“The long-term durability of FEVAR has been established, but its complexity may limit widespread adoption,” Starnes concluded. “Automated planning software provides an efficient and accurate way to identify fenestration locations for graft design.”
He continued, “Well planned FEVAR leads to high quality patient outcomes, and simplified FEVAR may benefit the majority of patients harbouring juxtarenal abdominal aortic aneurysms.”