Recent studies have shown the advantages of 3D printing for simulation of vascular surgery includes significant reduction of procedural time, but the applications of producing life-sized 3D printed models can have important educational benefits beyond the operation planning stage.
Bernhard Dorweiler of the University Medical Center in Mainz, Germany argued this point during the CX Innovation Showcase at the Charing Cross Symposium earlier this year (24–27 April, London, UK).
“3D printing is a revolutionary technique”, Dorweiler said, “that is increasingly being used in industry but also in medicine, predominantly for replacement of joints and bones.” At Dorweiler’s centre in Germany, 3D printing technology is now being used not only for the purpose of planning procedures with complex techniques or anatomies, but also as an important tool for education of residents as well as patients.
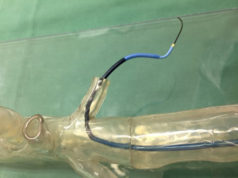
“We start by segmenting e.g. an aortic infrarenal aneurysm,” Dorweiler explained about the use of the technology in his own practice for training purposes. “We end up with a 3D electronic model of this aneurysm, and that dataset is then transferred to the 3D printer. There are several techniques and technologies for printing the file, but we are using a plastic polymer.” Once printed, the model is processed further to make the material transparent. This allows residents to practice a range of techniques, from cannulation to thoracic endovascular aortic repair (TEVAR), without any exposure to radiation.
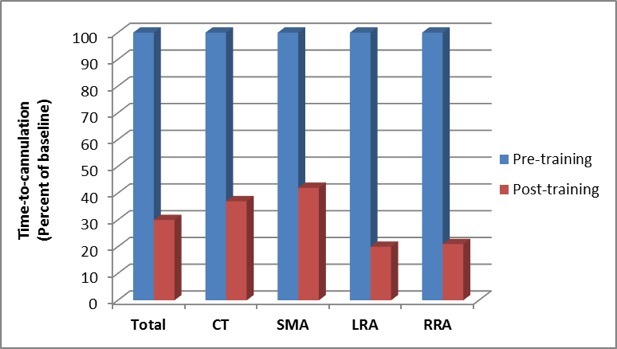
 “Using this 3D model for training of wire skills had some considerable improvements in the time need to cannulate the vessels,” Dorweiler said, “not only the superior mesenteric artery (SMA) but also the celiac trunk (CT) as well as left and right renal arteries (RRA; LRA).” The models are also used in the centre to practice the advancement and placing of a TEVAR graft without any imaging needed, which Dorweiler highlighted as a simple and important tool for a resident’s “first steps” in handling grafts and performing these procedures.
“Using this 3D model for training of wire skills had some considerable improvements in the time need to cannulate the vessels,” Dorweiler said, “not only the superior mesenteric artery (SMA) but also the celiac trunk (CT) as well as left and right renal arteries (RRA; LRA).” The models are also used in the centre to practice the advancement and placing of a TEVAR graft without any imaging needed, which Dorweiler highlighted as a simple and important tool for a resident’s “first steps” in handling grafts and performing these procedures.
 Recently, two studies have shown that using 3D printed models in vascular surgery to simulate a procedure for planning purposes reduces time in the operation room significantly: Torres et al’s study in the European Journal of Vascular and Endovascular Sugery (2017) observed a 30% reduction, while Tack et al’s paper in BioMedical Engineering OnLine (2016) found a mean reduction of 28 minutes. “This is a considerable advantage because it also shortens radiation exposure and postoperative morbidity,” Dorweiler noted.
Recently, two studies have shown that using 3D printed models in vascular surgery to simulate a procedure for planning purposes reduces time in the operation room significantly: Torres et al’s study in the European Journal of Vascular and Endovascular Sugery (2017) observed a 30% reduction, while Tack et al’s paper in BioMedical Engineering OnLine (2016) found a mean reduction of 28 minutes. “This is a considerable advantage because it also shortens radiation exposure and postoperative morbidity,” Dorweiler noted.
Models can be used in complex anatomies, as Dorweiler illustrated with a case of congenital malformation due to interrupted aortic arch in which numerous collaterals had formed which over time formed “a huge aneurysm in the chest and in the neck,” but 3D printing has also been used for new devices or strategies. Discussing one such case, Dorweiler said, “We printed a model because we wanted to implant of a double-branched graft. At the time, it was the first implantation of this graft (Bolton Medical) in Germany, so we wanted to look at whether the graft was able to be positioned in this dissection. We also took the postoperative CT scan and again segmented the implanted stent graft from this and generated 3D printed models.
“We were able to use both models not only to plan and simulate the procedure, but also to explain the anatomy to the patient. Having the anatomy in his hands, the patients was able to perceive what needed to be done and what has been done.”
A relatively new technology, particularly in terms of its applications in vascular surgery, 3D printed models currently leave some room for improvement. The process of creating a transparent model for training, with the polymer and printing technology used at this centre, means hardening the material. More true to life would be a polymer plastic material that is compliant as the walls of the aorta, but Dorweiler remains optimistic on this note, as he points out that industry is working on the problem and hopes they will soon have polymers that allow for both compliance and transparency.
Concluding the presentation, Dorweiler highlighted that by applying 3D printing technology in vascular surgery in simulation of complex anatomy and complex implants and training platforms for wire skills and graft placement, “we are able to achieve some OR time reduction and—most importantly—we are able to improve patient education and patient consent.”