Patrick Muck (Cincinnati, USA) examines some of the latest technologies available for radiation protection in the vascular space amid a “meteoric” rise in endovascular procedures.
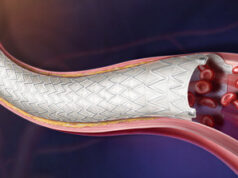
Over the past decade, the adoption of endovascular techniques has accelerated dramatically, driven by technological innovations, demographic shifts, and healthcare economics. However, this proliferation comes with challenges, particularly the heavy reliance on fluoroscopy for real-time imaging, which exposes healthcare providers to ionising radiation.
Globally, arterial procedures dominate endovascular volumes, comprising over 60% of hospital caseloads. Endovascular aneurysm repair (EVAR) for abdominal aortic aneurysms (AAAs) exemplifies this, with procedure volumes rising 25% from 2011 to 2016.1 In 2023–2024, lower limb revascularisation—primarily angioplasty and stenting for peripheral arterial disease (PAD)—saw a 45% increase, driven by below-the-knee therapies approved in early 2024. Peripheral vascular interventions (PVI) for PAD trended toward complexity, with tibial PVI usage up 1% annually and atherectomy 1.6% from 2011–2020, a pattern persisting into 2024.2 Office-based labs (OBLs) reported a dramatic uptick since 2008, performing complex arterial cases with lower costs.3 Carotid stenting procedures continue to increase as well.4
Venous procedures, though less voluminous than arterial, have seen robust expansion, focusing on chronic venous disease (CVD) affecting 30% of adults. Demographic factors, such as obesity and sedentary lifestyles, exacerbate venous issues, with projections estimating a 15% annual rise in CVD prevalence through 2030. Venous interventions have democratised treatment for lower extremity venous disease, affecting over 30 million Americans alone. The peripheral vascular devices market, heavily reliant on venous tools, is poised to expand from US$13.51 billion in 2025 to US$21 billion by 2032, at a compound annual growth rate (CAGR) of 6.5%.4 Training logs show venous cases rising from 25 to 43 per fellow annually (2007–2024), a statistically significant jump (p<0.001).5 In the UK, National Vascular Registry data indicate wait times for venous interventions stretched to 86 days in 2023, yet volumes grew amid rising CVD referrals.6 Venous procedures benefit from outpatient feasibility, with ambulatory surgical centre (ASC) volumes up 27% in 2023.4 Despite shorter fluoroscopy times than arterial counterparts, venous interventions still contribute to cumulative staff exposure.
Radiation mitigation spans procedural techniques, shielding, and innovative technologies. Protection starts with avoidance. As procedure volumes increase so do the occupational risks, prompting European Society for Vascular Surgery (ESVS) guidelines for ALARA, or As Low As Reasonably Achievable, strategies. The ALARA principle calls for reducing radiation to the patient, operator, and staff.7,8 Time, distance, and shielding are the cornerstones.7 Basic strategies include collimation and pulsed fluoroscopy.9 Personal protection with lead aprons, thyroid shields, and ceiling-suspended screens reduce scatter by 70–90%.10 Digital subtraction angiography (DSA) should be used judiciously during peripheral procedures.11,12 Personal dosimetry monitors should be worn by all operators and staff.8 Advanced systems such as Fiber Optic RealShape (FORS; Philips) use light-emitting guidewires for fluoroscopy-free navigation.13 Electromagnetic tracking and image fusion systems from Cydar Medical and Centerline Biomedical eliminate 20–40% of live fluoroscopy needs.14,15 Traditional lead aprons reduce exposure by 70–90% but cause musculoskeletal strain and orthopaedic concerns. Recently, scatter control and barrier protection systems have been developed to dramatically reduce radiation exposure to team members. Radiaction and EggNest target scatter control whereas Protego and Rampart offer barrier protection. Radiaction and Protego are more aimed for cardiac procedures, while EggNest Complete and Rampart are more applicable to the peripheral vascular space and will be highlighted for this readership.
The EggNest Complete system (Egg Medical) is an integrated radiation protection system designed to integrate into the existing workflow of any fluoroscopy suite. Its modular design allows for easy integration for multiple vascular and cardiovascular case types. The retractable shielding and unique modular design allow for full lateral and bi-plane use as well. The EggNest Complete system is comprised of carbon fibre and nonlead equivalent panels above the table, flex shielding below the table, and a large ceiling-mounted shield. The patented shielding easily integrates into existing rooms and offers total team protection without taking up valuable floor space in crowded surgical suites. A 2025 real-world study presented at the Transcatheter Cardiovascular Therapeutics (TCT) meeting (25–28 October; San Francisco, USA) showed that the EggNest Complete total operator dose was incredibly low at 0.16mRem, meaning that the operator could do 31,000 cases in a year before reaching their annual allowable dose limit.
The EggNest portfolio also includes the EggNest Protect, which is similar to the EggNest Complete, but without the ceiling-mounted shield. Clinical data presented at the 2025 Western Vascular Society (WVS) annual meeting (14–17 September; Ojai, USA) by Brant Ullery (Providence St Joseph Health, Portland, USA) utilising the EggNest Protect (without the ceiling-mounted shield) demonstrated a 97.4% reduction in radiation exposure across 27 complex multivessel aortic cases for every person in the procedure room.16
The Guardian is Rampart’s latest innovation in their suite of radiation safety solutions and represents a paradigm shift in occupational protection, offering comprehensive, total room protection via modular, ceiling- or floor-mounted panels that block scatter radiation at its source. Unlike traditional lead aprons, Guardian deploys transparent, lightweight shields engineered from proprietary composite materials that are completely lead-free. In a recent randomised controlled trial, the Rampart system demonstrated greater than 99% attenuation, a 20-fold reduction in total body radiation when compared to standard lead aprons and shields.17
Guardian integrates seamlessly with C-arms, allowing 360-degree rotation without repositioning. In a 2025 study of peripheral vascular cases, Guardian reduced effective doses from 2–5mRem to under 0.1mRem per procedure, addressing head and extremity exposure where lead aprons provide limited protection. Real-world data from high-volume centres show 40% fewer orthopaedic complaints among users, as the system eliminates apron weight (up to 20lbs).18 Cost-effectiveness stems from durability—shields last 10+ years—and reduced absenteeism. In recognition of this new era in radiation safety devices, societies such as the Society for Cardiovascular Angiography & Interventions (SCAI) and the Society for Vascular Surgery (SVS) have recently come together to write a consensus document to be published in Q1 that further discusses the role of Enhanced Radiation Protection Devices (ERPDs). At my institution, the last five EVARs with the Guardian have recorded a combined exposure of less than 2.1mRem—less than one receives on a coast-to-coast flight in the USA. In fact, the exposures were so low, in two of the EVARs, the entire team was lead apron free.
The meteoric rise of endovascular procedures—arterial and venous alike—ushers in an era of precise, patient-friendly care, yet underscores the imperative for radiation stewardship.19 A new era of barrier protection has arrived and it’s our generation’s duty to protect patients and the entire team.19 As endovascular volumes grow 7% yearly, prioritising these barrier technologies safeguards the workforce. Protego and Radiaction are efficacious for the cardiology space, whereas Rampart’s Guardian and EggNest Complete are incredibly effective in the peripheral vascular space. Rampart’s Guardian and EggNest Complete redefine mitigation, blending efficacy, ergonomics, and equity to combat radiation’s hidden toll.
References
- Guez D, Hansberry DR, Gonsalves CF, et al. Recent trends in endovascular and surgical treatment of peripheral arterial disease in the Medicare population. AJR Am J Roentgenol. 2020 May; 214(5): 962–966. doi: 10.2214/AJR.19.21967. Epub 2020 Feb 25. PMID: 32097027.
- Dun C, Stonko DP, Bose S, et al. Trends and factors associated with peripheral vascular interventions for the treatment of claudication from 2011 to 2022: a national Medicare cohort study. J Am Heart Assoc. 2024 Jul 16; 13(14): e033463. doi: 10.1161/JAHA.123.033463. Epub 2024 Jul 3. PMID: 38958132; PMCID: PMC11292772.
- Cook R, Robbins J, Truax L, Hingorani A. Patient selection for arterial procedures in office-based laboratories: a systematic review. Semin Vasc Surg. 2024 Jun; 37(2): 118–132. doi: 10.1053/j.semvascsurg.2024.05.003. Epub 2024 May 21. PMID: 39151992.
- Vascular surgery and endovascular procedures market size, share, growth, and industry analysis, by type (open surgery, endovascular procedures), by application (hospitals, ambulatory surgical centers, specialty clinics), regional insights and forecast to 2033. https://www.marketgrowthreports.com/market-reports/vascular-surgery-and-endovascular-procedures-market-114587#:~:text=The%20%22Vascular%20Surgery%20and%20Endovascular,endovascular%20care%20across%2080%20countries.
- Roth A, Moreno O, Santos T, et al. Impact of the endovascular revolution on vascular training through analysis of national data case reports. J Vasc Surg. 2024 Jun; 79(6): 1498–1506.e12. doi: 10.1016/j.jvs.2024.01.207. Epub 2024 Feb 15. PMID: 38367849.
- National Vascular Registry State of the Nation Report 2024
- Modarai B, Haulon S, Ainsbury E, et al. Editor’s Choice – European Society for Vascular Surgery (ESVS) 2023 clinical practice guidelines on radiation safety. Eur J Vasc Endovasc Surg. 2023 Feb; 65(2): 171–222. doi: 10.1016/j.ejvs.2022.09.005. Epub 2022 Sep 18. PMID: 36130680.
- Chambers CE, Fetterly KA, Holzer R, et al. Radiation safety program for the cardiac catheterization laboratory. Catheter Cardiovasc Interv. 2011 Mar 1; 77(4): 546–56.
- Ketteler ER, Brown KR. Radiation exposure in endovascular procedures. J Vasc Surg. 2011 Jan; 53(1 Suppl): 35S–38S. doi: 10.1016/j.jvs.2010.05.141. Epub 2010 Sep 16. PMID: 20846817.
- Meisinger QC, Stahl CM, Andre MP, et al. Radiation protection for the fluoroscopy operator and staff. AJR Am J Roentgenol. 2016 Oct; 207(4): 745–754. doi: 10.2214/AJR.16.16556. Epub 2016 Jul 19. PMID: 27440524.
- Haqqani OP, Agarwal PK, Halin NM, et al. Minimizing radiation exposure to the vascular surgeon. J Vasc Surg. 2012 Mar; 55(3): 799–805.
- Meisinger QC, Stahl CM, Andre MP, et al. Radiation protection for the fluoroscopy operator and staff. AJR Am J Roentgenol. 2016 Oct; 207(4): 745–54.
- Sanders AP, Swerdlow NJ, Jabbour G, Schermerhorn ML. The effect of Fiber Optic RealShape technology on the reduction of radiation during complex endovascular surgery. J Vasc Surg. 2024 Apr; 79(4): 954–961. doi: 10.1016/j.jvs.2023.11.002. Epub 2023 Nov 4. PMID: 37931886; PMCID: PMC10960673.
- Malkoc A, Gnanadev R, Shoemaker HB, et al. The use of advanced three-dimensional computed tomography during simple and complex endovascular aortic aneurysm repairs. Ann Vasc Surg. 2024 Sep; 106: 90–98. doi: 10.1016/j.avsg.2024.03.004. Epub 2024 May 14. PMID: 38754579.
- Farivar BS. Advanced intraprocedural image guidance for endovascular aortic and branch-vessel procedures using the Intraoperative Positioning System (IOPS). Semin Intervent Radiol. 2024 Dec 18; 41(6): 570–575. doi: 10.1055/s-0044-1800958. PMID: 40190771; PMCID: PMC11970956.
- Ullery BW, Lee JT, Han SM. Next generation radiation reduction technology in complex endovascular aortic surgery: protecting the entire interventional team. Presentation presented at Western Vascular Surgical Society meeting; September 2025; Ojai, USA.
- Lisko JC, Shekiladze N, Chamoun J, et al. Radiation exposure using Rampart vs standard lead aprons and shields during invasive cardiovascular procedures. J Soc Cardiovasc Angiogr Interv. 2023 Oct 19; 3(1): 101184. doi: 10.1016/j.jscai.2023.101184. PMID: 39131978; PMCID: PMC11308832.
- Herzig MS, Kochar A, Hermiller JB, et al. Real-world reductions in lead-free radiation exposure with the Rampart system during endovascular procedures. Am J Cardiol. 2025 May 15; 243: 59–64. doi: 10.1016/j.amjcard.2025.02.019. Epub 2025 Feb 20. PMID: 39986445; PMCID: PMC11972878.
- Rizik D, Sutton NR, Alasnag M, et al. SCAI/ASE/HRS/SIR/SVS expert consensus statement on enhanced radiation protection: time for mandatory and urgent action. J Soc Cardiovasc Angiogr Interv. 2025; In press. doi:10.1016/j.jscai.2025.103597.
Patrick E Muck is chief of vascular surgery at the Good Samaritan Hospital in Cincinnati, USA.
The author declared no relevant disclosures.