Peripheral artery disease patients who undergo endovascular treatment may have a lower risk of major and life-threatening bleeding events and a lower risk or restenosis or occlusion when treated with edoxaban and aspirin, rather than with clopidogrel and aspirin, according to a new proof of concept study.
Frans Moll, University Medical Centre, Utrecht, The Netherlands, presented the data on behalf of the ePAD (Edoxaban in peripheral arterial disease) study steering committee and investigators.
Research gains have improved operator skill and device performance in peripheral endovascular techniques. However, there has been limited research in medical therapy following peripheral endovascular procedures. According to Moll, guideline recommendations still vary significantly, ranging from the use of aspirin alone to the use of clopidogrel with aspirin for one to three months followed by continued long-term aspirin use. Treatment recommendations focus on platelet aggregation, and exclude the role of the coagulation cascade in thrombus formation.
Loss of patency after endovascular treatment remains high, ranging from 17–>40% with dual antiplatelet therapy. Endovascular treatment can also result in catheter-induced damage to the endothelium, exposing tissue factor-rich subendothelium to the blood stream and creating a thrombogenic environment wherein platelets and coagulation factors are activated.
Moll told delegates that the development of a regimen that targets all major components of the arterial thrombi may help preserve patency restored by endovascular techniques in peripheral artery disease patients with a low risk of bleeding. In this trial, Moll and colleagues compared the combination of edoxaban (Lixiana/Savaysa, Daiichi Sankyo) and aspirin with conventional dual antiplatelet therapy treatment (clopidogrel with aspirin) in maintaining post-femoropopliteal endovascular therapy vessel patency in peripheral artery disease patients. Moll noted that this “is the first study to utilise a non-vitamin K antagonist oral anticoagulant in a dual antithrombotic regimen in peripheral artery disease patients.”
The 200 enrolled US and European patients all exhibited peripheral artery disease with Rutherford class 2–5 and had undergone successful endovascular treatment (≤30% residual stenosis) in the superficial femoral artery and for proximal popliteal lesions. They were randomised 1:1 to the two groups and follow-up visits were scheduled for one, two, three, four and six months. Patients with active bleeding or high bleeding risk or with creatine clearance <30mL/minute were excluded, as were patients with ongoing indications for dual antiplatelet therapy or anticoagulant treatment.
Patient characteristics were similar at baseline. Around 70% of patients in both groups had Rutherford classification of 3 or higher, indicating severe claudication. Lesion length was ≥7cm in around 60% of patients in both groups, stenosis was observed in approximately 64% of both groups and occlusion in approximately 35% of both groups—“serious pathology,” Moll said.
The study’s primary safety endpoint was focused on adjudicated bleeding using TIMI and ISTH criteria, and primary efficacy endpoint was restenosis or reocclusion at six months, defined as peak systolic velocity ratio ≥2.4 at the treated segment obtained using duplex ultrasonography.
Edoxaban with aspirin showed lower incidence of major bleeding (0) and any bleeding (5) compared with clopidogrel (major bleeding=2, any bleeding=9) as measured by TIMI criteria. ISTH criteria non-major bleeding (11 vs 8) and any bleeding (30 vs 28) were higher with edoxaban and aspirin than clopidogrel and aspirin, though major bleeding was lower (1 vs 5).
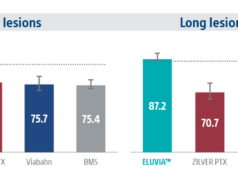
Six-month composite endpoint event rates showed that edoxaban was a more favourable treatment than clopidogrel in all events of restenosis/reocclusion, with or without target lesion revascularisation, amputation and/or major adverse cardiac events. It was also the more favourable treatment for all different patient characteristics including gender, lesion length, age and region.
Given these encouraging results, Moll told the audience that “an adequately sized trial will be needed to confirm this potentially paradigm shifting treatment approach”.