The results of a small-scale pilot study from Asia have indicated “potentially disappointing” results with a novel drug-eluting balloon in treating dysfunctional arteriovenous access for dialysis. These findings were delivered by Tjun Tang (Singapore General Hospital, Singapore)—who also highlighted “excellent” technical and clinical success rates and positive safety outcomes—via a Podium 1st presentation at the 2022 Charing Cross (CX) International Symposium (26–28 April, London, UK).
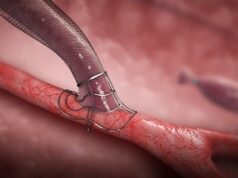
Tang presented 12-month results from the ISABELLA (Intervention with Selution SLR agent balloon for endovascular latent limus therapy for failing AV fistulas) trial, which assessed the utility of the Selution SLR sirolimus-eluting balloon (MedAlliance) for minimising the effect of neointimal hyperplasia and treating arteriovenous fistula (AVF) stenosis.
The speaker noted that ISABELLA had a recruitment target of 40 patients, with 34 of these patients (85%) ultimately being evaluated at the 12-month follow-up timepoint in November 2021. He also detailed that the majority of these patients had either radiocephalic or brachiocephalic fistulas with recurrent lesions requiring treatment—and the most common indication for intervening was a drop in access flow, observed in 61.5% of cases.
Moving on to 12-month data from the trial, Tang reported a target-lesion primary patency (TLPP) rate of 44% (16/36 lesions) and a circuit access patency rate of 31% (10/32 lesions), which represented decreases from 72% and 63%, respectively, at six months. In addition, he stated that the overall rate of secondary patency—defined as freedom from access circuit abandonment—was 94.1% (32/34 patients) at 12 months compared to the 97.2% (35/36 patients) observed at six months.
“In conclusion, the ISABELLA study showed excellent technical and clinical success rates [100%],” Tang said.
He also relayed that the use of Selution SLR in patients with AVF stenosis appears safe, with no serious adverse events, such as pulmonary embolism or bronchopneumonia, being associated with its use in the study. And, in terms of efficacy, Tang added that—while the results are “potentially disappointing”—this is a small, exploratory study and alluded to possible confounding factors within these findings.
“We do need longer-term data and randomised controlled studies […] if we are going to move forward seriously within this field, and with this technology,” Tang concluded. And, speaking to Vascular News, Tang noted the importance of being careful when interpreting the results of an exploratory pilot study—especially one that was designed to power a randomised controlled trial, as this one has been.
“I do not think it is actually a setback at all,” he continued. “In fact, I think it is very encouraging. I think the fact we are not getting any serious adverse events with the balloon […] is reassuring.”
Tang also told Vascular News that, with the exception of the IN.PACT AV Access study (Medtronic), a similar drop-off in patency rates between six and 12 months had been observed in several previous studies using paclitaxel to treat dysfunctional dialysis access.